Helping to stop colorectal cancer by identifying metastasis chances early

Colorectal cancer, one of the most commonly diagnosed cancers in the United States, is not a commonly discussed disease. Often symptomless in early stages, the cancer is more difficult to treat as it progresses, requiring chemotherapy in later stages. Researchers at the University of Notre Dame are working on a way to identify patients who would benefit from chemotherapy before the cancer progresses.
Amanda Hummon, Huisking Foundation Inc. Associate Professor of Chemistry and Biochemistry, and Steven Buechler, professor of applied and computational mathematics and statistics, have used their cross-disciplinary backgrounds to help researchers understand the risk of cancer relapse or metastasis for Stage II colon cancer patients.
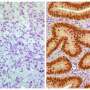
Many people understand that colorectal cancer develops in the colon or rectum, which is also known as the large intestine. What people may not realize is that the large intestine actually has two different sections: the right side (ascending and transverse colon) and the left side (from the descending colon to the rectum). The two sides of the colon fuse together during embryogenesis—the early stages of prenatal development—to form the large intestine, which causes the two sides to have different protein expressions. Buechler and Hummon are using this information to find a way to identify Stage II cancer patients who are more likely to develop metastasis.
In traditional colon cancer treatment, chemotherapy isn't recommended until the cancer has progressed to Stage III or higher. Ideally, Hummon and Buechler's test will enable the clinical team to determine which patients with the early stages of the disease are likely to benefit from more aggressive treatment versus those who do not need strong chemotherapy. Patients will therefore be spared from the side effects of treatment if they are unlikely to benefit from it.
"Professor Hummon and I have been mapping gene expressions for the right versus the left side of the colon, which we now know are different from each other due to the way the colon forms," said Buechler. "With this information we are developing a prognostic test to help people with Stage II colorectal cancer know if they are likely to develop a metastasis. With this knowledge they may be able to request treatment, even if it is not typically recommended at this early stage."
For the test, Buechler and Hummon analyze a biopsy from a Stage II colon cancer tumor. Then—noting the side of the colon that the tumor originated from—the researchers look at gene expression. Based on how the genes fit within the original, mapped profile, they can predict with a high accuracy if a particular patient will develop metastatic tumors.
"We are looking specifically at Stage II colon cancer patients due to the risk associated with standard treatment plans and the need for personalized care," said Hummon. "Currently, 25 percent of Stage I and Stage II patients will develop a metastasis. If this test is successful on a broad scale, the goal is to lower cancer recurrence for colorectal patients."