March 25, 2016 report
Promising treatment for flu-related lung injury
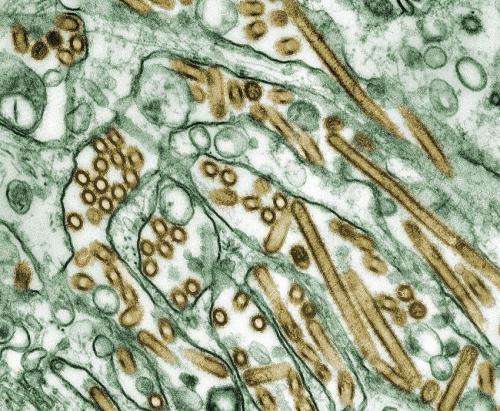
(Medical Xpress)—Influenza is highly communicable, and often causes acute lung injury and respiratory distress, particularly in aged people. Therapeutic options after infection with the virus are limited, and health organizations emphasize vaccination and sanitary measures to prevent the spread of flu viruses. Additionally, antiviral therapy does not always reduce acute lung injury, and medical researchers are keen to find new approaches.
An international group of researchers recently published the results of a study in the Proceedings of the National Academy of Sciences that treated H5N1-infected mice with multipotent mesenchymal stromal cells (MSCs), which significantly reduced the impairment of fluid clearance from the alveoli and prevented or reduced acute lung injury. In fact, the results of this mouse trial were so remarkable that the authors wrote, "This potential adjunctive therapy for severe influenza-induced lung disease warrants rapid clinical investigation."
The H5N1 and H7N9 viruses target lung epithelial cells—this is the gas exchange interface where oxygen becomes available to the blood supply. These cells are also responsible for transporting water, sodium and chloride away from the apical surface of the alveolar epithelium; when this process is impaired, the result is acute lung injury.
Observing that MSCs have beneficial therapeutic effects for lung injuries resulting from other types of bacterial and viral illnesses, the researchers studied the effects of MSC treatment on two flu viruses, H5N1 and H1N1. In the course of their study, the researchers discovered that H5N1 dysregulates alveolar fluid clearance and protein permeability by causing the down-regulation of the lung's alveolar sodium and chloride transporters.
They write, "When we cocultured alveolar epithelium with MSCs, these injury mechanisms were prevented or reduced." This led them to attempt treating mice infected with H5N1, which resulted in a "clinically significant reduction in lung pathology and increased survival in association with a modulation of these pathogenic mechanisms in vivo."
The H5N1 and other viruses induce the alveolar epithelium to produce factors that down-regulate its ability to clear fluid from the lungs; the seasonal H1N1 virus does not have this effect on the epithelium, and mice infected with H1N1 did not have the same therapeutic results. Additionally, the MSC treatment was only effective in older mice, those eight to 12 months old. Results were not significant in younger mice aged six to eight weeks.
The authors note that aged animals have lower expression of genes involved in cell activation and migration of cytokine and chemokine receptors. "Thus, younger animals have more potent endogenous MSC responses, whereas exogenous MSC therapy is more likely to exert an apparent benefit in older animals," they write.
They also note that the goal of their study was to determine the impact of MSC therapy on the progression of severe infection; they recommend that future studies examine the interactions of MSCs with antivirals, and that researchers further investigate the effects of age on MSC therapy.
More information: Human mesenchymal stromal cells reduce influenza A H5N1-associated acute lung injury in vitro and in vivo. PNAS 2016 ; published ahead of print March 14, 2016, DOI: 10.1073/pnas.1601911113
Abstract
Influenza can cause acute lung injury. Because immune responses often play a role, antivirals may not ensure a successful outcome. To identify pathogenic mechanisms and potential adjunctive therapeutic options, we compared the extent to which avian influenza A/H5N1 virus and seasonal influenza A/H1N1 virus impair alveolar fluid clearance and protein permeability in an in vitro model of acute lung injury, defined the role of virus-induced soluble mediators in these injury effects, and demonstrated that the effects are prevented or reduced by bone marrow-derived multipotent mesenchymal stromal cells. We verified the in vivo relevance of these findings in mice experimentally infected with influenza A/H5N1. We found that, in vitro, the alveolar epithelium's protein permeability and fluid clearance were dysregulated by soluble immune mediators released upon infection with avian (A/Hong Kong/483/97, H5N1) but not seasonal (A/Hong Kong/54/98, H1N1) influenza virus. The reduced alveolar fluid transport associated with down-regulation of sodium and chloride transporters was prevented or reduced by coculture with mesenchymal stromal cells. In vivo, treatment of aged H5N1-infected mice with mesenchymal stromal cells increased their likelihood of survival. We conclude that mesenchymal stromal cells significantly reduce the impairment of alveolar fluid clearance induced by A/H5N1 infection in vitro and prevent or reduce A/H5N1-associated acute lung injury in vivo. This potential adjunctive therapy for severe influenza-induced lung disease warrants rapid clinical investigation.
© 2016 Medical Xpress










.jpg)





