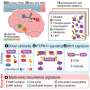
How diet influences our genes

What we eat can directly affect the genetic programs that regulate cellular function. A new EU project, coordinated by an LMU researcher, will explore how the products of metabolism intervene in gene regulation.
The incidence of chronic illnesses such as obesity, diabetes and high blood pressure has already reached alarmingly high levels. Often collectively referred to as metabolic syndrome, these disorders are ultimately attributable to perturbations in biochemical metabolism, and all are caused by a combination of lifestyle factors, unbalanced diet and genetic influences. However, genes do not rigidly determine how an organism processes its food. On the contrary, recent evidence indicates that intermediates produced during the biochemical reactions involved in the breakdown of nutrients can themselves have an impact on gene regulation. – Indeed, cells can actually be reprogrammed by such substances. "Much of what we eat is directly converted into metabolic products that play a part in controlling the action of our genes," says Professor Andreas Ladurner, who works at the LMU's Biomedical Center. In a new EU-funded Innovative Training Network (ITN) for PhD students called ChroMe (Chromatin & Metabolism), which will be coordinated by Ladurner, an international team of researchers plans to identify the molecular mechanisms that account for these emerging connections between genes and nutrition, and will search for targeted approaches to the therapy of the metabolic syndrome.
The genomic DNA carried by each cell encodes the information necessary for the synthesis of the different proteins produced by a given tissue and organ. In higher organisms, the hereditary material resides in the cell's nucleus in a compact form known as chromatin, which results from the interaction of the long DNA molecules with a set of proteins called histones. Which genes are activated or repressed in a given cell is in part determined by so-called epigenetic modifications of the chromatin. These are comparatively simple chemical tags that serve as molecular switches – and it is these marks that are now known to be modulated by diet. "The long-term consumption of excessive amounts of sugar and alcohol, for example, leads to drastic reprogramming of cells in the liver and other tissues, and these changes in gene regulation can promote the development of obesity and the loss of sensitivity to insulin," says Ladurner. Other studies carried out by some of the groups involved in ChroMe have shown that other elements of lifestyle - such as exercise - as well as factors in our physical environment, can modulate the composition of our gut microflora, which in turn have an impact on gene activity in our cells.
These new insights point to previously unappreciated targets for the effective treatment of metabolic diseases. "However, we still know relatively little about the molecular and physiological mechanisms that mediate the interactions between diet and gene regulation," Ladurner points out. Hence, the primary objective of ChroMe is to elucidate these mechansims. The participating researchers and their doctoral students will investigate in particular how enzymes involved in the epigenetic modification of chromatin are affected by dietary components and, conversely how epigenetic marks alter metabolic processes and general physiology.