Does where you live play a role in your life expectancy?
The gap in lifespan between the rich and the poor has grown rapidly in recent years, with the richest Americans gaining three years since 2000 but the poorest gaining none. Moreover, there is a disparity in lifespan based on where the poor live. The findings come from new research by the Health Inequality Project published online in the Journal of the American Medical Association on Sunday.
We asked Daniel Kim, associate professor in the Bouvé College of Health Sciences, to comment on what's driving the lifespan disparity from city to city, why place of residence influences longevity for the poor but not the rich, and what the new findings might mean regarding the way public health leaders and policymakers address the issues of health and income inequality.
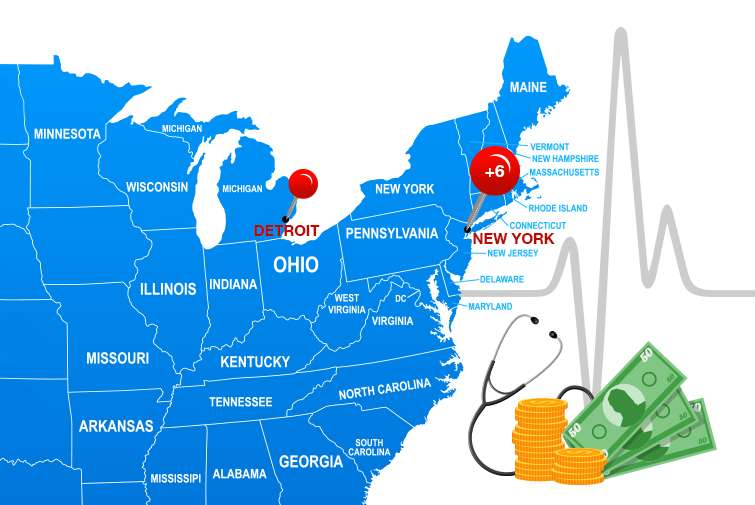
The JAMA study reports that there is a disparity in lifespan based on where the poor live, not just between the rich and poor. For example, life expectancy for the very poor in New York is six years longer than it is in Detroit, and the poor in certain cities—including New York, Los Angeles, and Birmingham, Alabama—live nearly as long as their better-off neighbors. Why is that, and do those results surprise you?
These findings are not surprising to many of us in my field of social epidemiology who think about and investigate multiple social, physical, and economic determinants at a population level. We know that there are enormous variations in the types of societal conditions in which people are born, grow, live, work, and age, especially in a country as vast as the U.S. with such a diverse population. These societal conditions extend beyond one's income and are related to the policies and people that characterize these places, as well as other physical and environmental characteristics. For example, cities like New York may have policies in place such as smoking bans, soft drink size limit, or environmental policies concerning lead levels in drinking water that are better for health and can benefit all individuals living within those cities, including the very poor. There may also be higher levels of government spending on programs and services, such as welfare and social services, within these cities—and such social spending may be beneficial to health, as the results of my recently published study suggest. Finally, there may also be positive benefits called spillover effects by virtue of living in close proximity to rich residents, who are able to bring about or maintain the presence of more economic and material resources for the city, including better kept parks for leisure and employment opportunities, and who may also possess healthier behaviors, which in turn may influence the behaviors of nearby poorer residents. These are all plausible explanations, but they have yet to be formally researched.
The study notes that the gap in lifespan between rich and poor grew from 2001 to 2014: Among American men, those with incomes in the top 1 percent live 15 years longer than the poorest men, while the women in the top 1 percent live 10 years longer than the poorest women. Why does place of residence not make a difference regarding longevity for the rich while it makes a significant difference for the poor?
According to the study, there was a larger increase in life expectancy observed for higher income groups during the 2000s. The results of the study's time trend analysis over the period from 2001 to 2014 tell us that the rich benefit more than the poor. This would be entirely consistent with the study's findings of an association between income and life expectancy if the incomes of the rich are increasing at a faster rate than those of the poor over time. This is indeed what has been happening. According to the U.S. Congressional Budget Office, between 1979 and 2007, after-tax incomes grew by 275 percent for the top 1 percent of households; by 65 percent for the next 19 percent; by just under 40 percent for the next 60 percent; and by only 18 percent for the bottom 20 percent. Other research, using the data from the National Longitudinal Mortality Study, similarly found a widening of the life expectancy gap by education in the 1980s and 1990s, whereby virtually all gains in life expectancy occurred only among the highly educated groups. So overall, this presumed effect of income on health at an individual level is fully in keeping with what is captured and seen in the researchers' aggregate analysis at the level of location.
Public health leaders and policymakers have focused a great deal of attention on income inequality as the driver behind the differences in lifespan for rich and poor. How might these findings change how they address the issues of health, mortality, and income inequality?
As a population health driver, the jury is still out on income inequality, and I don't believe that this study alone can render a verdict or give us strong insights for policy. I would point to some of the scientific shortcomings of this study, including that it focused on "commuting zones" as the geographic level of analysis. These spatial units are on the order of the size of entire cities, which can be extremely large, like New York City. In my field of epidemiology, we refer to such a study design as "ecological," meaning that the ability to make inferences about cause-and-effect relationships, especially at an individual level, is limited. This is also expressed by the phrase "correlation does not equal causation." In particular, there may be characteristics that differ between places that could confound the associations found, and there may also be differences in the characteristics of people that inhabit these different places. And unless we are able to fully control for all of these factors, we cannot disentangle and identify what is truly cause and effect. So while the study found a correlation between income inequality and average life expectancy across commuting zones (which is consistent with an income inequality effect), and observed that most of this correlation may be due to places with more income inequality having a higher percentage of low-income people (which argues against an income inequality effect), we are still plagued by the issue of confounding variables and are unable to make good causal inferences. In addition, it should be noted that this study focused on pre-tax income rather than after-tax income. If the effects on life expectancy are due to an absolute income effect only, and not also due to relative income (that is, income inequality), we would expect to see similar patterns hold up if the researchers had used after-tax income. Unfortunately, even with such an analysis, which might lend greater support for an effect of income inequality on health, there would still be more questions raised than answered if the same study design were used.
More information: Raj Chetty et al. The Association Between Income and Life Expectancy in the United States, 2001-2014, JAMA (2016). DOI: 10.1001/jama.2016.4226



















