Genetic target could help fight deadly drug-resistant infections
Fungal infections pose a major threat to hospital patients and have proven difficult to combat, but scientists have unlocked evidence that could lead to more effective treatment.
Researchers at The Ohio State University are the first to identify a potential gene-based approach to increasing the immune response to the fungus Candida albicans, which can find its way into the bloodstream and vital organs, including the kidneys. Tests of a potential treatment approach in mice rescued the animals from death.
Invasive Candida infection is one of the leading causes of hospital-acquired bloodstream infections, which carry a mortality rate ranging from 45 to 75 percent.
"Catheterized patients - especially those with cancer who receive chemotherapy and those with an organ transplant who receive immunosuppressive treatment - are highly susceptible to these infections, which can be lethal," said lead researcher Jian Zhang, an associate professor of microbial infection and immunity.
"We've found a potential way to manipulate the immune system to treat invasive, life-threatening cases that are resistant to treatment," he said.
The research appears in the journal Nature Medicine.
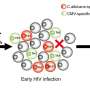
When they began their study, Zhang and his team knew that a group of molecules called C-type lectin receptors play a key role in controlling fungal infections. In healthy individuals whose bodies fight off the infection, these receptors detect the bad fungal cells and set off a chain of events that kicks the immune system into action.
Through previous work, the researchers knew that a gene called CBLB played a role in the process, but just what role was unclear.
Through tests of human cells in petri dishes and in mice, Zhang's group was able to pinpoint what CBLB does. CBLB targets two proteins (dectin 1 and 2), which send messages crucial for a robust immune response. The dectin proteins' job is to recognize the carbohydrates that line the fungi's cell wall and kick off an appropriate response by immune cells.
In a perfect scenario, CBLB's role is to guard against a too-intense immune response to the Candida infection. It tamps down inflammation and prevents tissue damage by moving proteins to a molecular "trash can," Zhang said.
But in weak hospitalized patients with bloodstream infections, CBLB stands in the way of an optimal immune response, Zhang said. In these patients, the immune response is dampened to a level that no longer protects patients against fungal invaders.
Through their work in mice, the researchers confirmed that if they knocked out CBLB function either through eliminating or deactivating it, the animals' immune systems waged a greater battle against the yeast.
"Ideally if you can downregulate or inactivate the gene, the antifungal response will be accelerated so you can clear the infection," Zhang said.
His team confirmed this in mice by injecting "small interference RNA" in an attempt to interrupt CBLB expression. Then they injected Candida albicans 24 hours later.
"We found when we do it this way, we can actually rescue the mice from death."
That opens the door to further research exploring the possibility of a gene-based treatment for humans that would target CBLB to allow patients' immune systems to effectively tackle the invader, Zhang said.
More information: Targeting CBLB as a potential therapeutic approach for disseminated candidiasis, Nature Medicine , nature.com/articles/doi:10.1038/nm.4141