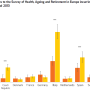
Internists say cost sharing, particularly deductibles, may cause patients to forgo or delay care
The American College of Physicians (ACP) today said that cost sharing, particularly deductibles, may cause patients to forgo or delay care, including medically necessary services. "The effects are particularly pronounced among those with low incomes and the very sick," said Nitin S. Damle, MD, MS, FACP, president of ACP.
"Addressing the Increasing Burden of Health Insurance Cost Sharing," ACP's most recent position paper, was released today by the 148,000-member organization.
"Underinsurance is emerging as a serious problem that may be more difficult to tackle than un-insurance," Dr. Damle said. "Evidence shows that when cost sharing is imposed, consumers may respond by reducing their use of both necessary and unnecessary care."
ACP's asserts that a different cost-sharing approach is needed to ensure that vulnerable people can afford medically necessary care in the face of rising health coverage costs and stagnant wages.
The five recommendations in the paper address ways cost sharing can be made more equitable in the private market by reducing overall health care spending, designing insurance plans that allow access to high-value services, enhancing financial subsidies for marketplace-based insurance plans, improving outreach and health insurance literacy and education, and advocating for updated research on the effects of patient cost sharing. They are:
- Helping contain health insurance premiums and cost sharing, the health care system must accelerate its efforts to reduce overall health care spending in ways that do not rely principally on shifting the cost burden onto insured persons who cannot afford to pay more for their medical care.
- Encouraging use of high-value health care:
- Consider implementing value-based insurance design strategies that reduce or eliminate out-of-pocket contributions for services proven to offer the greatest comparative benefit, with higher cost-sharing for services with less comparative benefit. Such strategies should be based on rigorous comparative effectiveness research by independent and trusted entities that do not have a financial interest in the results of the research. The goal should be to ensure that high-value cost-sharing strategies encourage enrollees to seek items and services proven to be of exceptional quality and effectiveness and not just on the basis of low cost;
- Consider implementing income-adjusted cost-sharing approaches that reduce or directly subsidize the expected out-of-pocket contribution of lower-income workers to avoid creating a barrier to their obtaining needed care.
- Improving cost-sharing provisions under the Patient Protection and Affordable Care Act.
- Working together among stakeholders to enhance health insurance literacy and promote better, more accessible, and objective information about cost-sharing requirements and health insurance plan design.
- Implementing a large-scale demonstration to test the short- and long-term effects of cost sharing in different populations.
"An alternative approach is needed to reduce spending through systemic reform of the health-care sector, protect low-income workers from overly burdensome out-of-pocket costs, enhance subsidies for marketplace Quality Health Programs, increase health care literacy, and direct shoppers to the right type of plan so that patients are shielded from financial ruin and insurance can function as intended," Dr. Damle concluded. "ACP has provided that today with this position paper."
More information: www.acponline.org/acp_policy/p … ost_sharing_2016.pdf