Simple procedure could improve treatment for common eye disease
A new, minimally invasive procedure appears to be effective for many patients with Fuchs endothelial dystrophy (FED), a common eye disease, without the potential side effects and cost of the current standard of care, a cornea transplant.
In a proof-of-concept study, published in the journal Cornea, researchers led by Kathryn Colby, MD, PhD, the Louis Block professor and chairman of the Department of Ophthalmology and Visual Science at the University of Chicago, showed that removing a few square millimeters of a single layer of cells on the inside of the cornea allowed rejuvenation of the surrounding tissue, without the need for a corneal transplant. This simple procedure restored clear vision to three out of four patients suffering from FED, the most frequent cause for corneal transplantation in the United States.
Over the past two years while at Harvard Medical School, Colby performed the new procedure, known as Descemet stripping, on 11 patients, aged 51 to 91. Two patients had the procedure in both eyes, one at a time.
When assessed six months after the operation, ten of the treated eyes (77 percent) had clear corneas and eight had 20/20 vision or better (two patients had retinal disease that limited their final vision). The other three eyes did not respond and required a standard cornea transplant.
"It's too soon to call this a cure," Colby said. "We performed the first operation just over two years ago. But when it works, it's a wonderful thing. It's quick, inexpensive and it spares patients from having someone else's cells in their eyes, which requires local immunosuppression."
The first patient to undergo Descemet stripping, 69-year-old Eric Thorp of the Boston area, was pleased. "It's quite a breakthrough," he said. His vision, now 20/20 in that eye, "is equivalent to what I had as a boy," he said. "Amazing."
"It's kind of an honor to have been the first," he added. "It was worth doing."
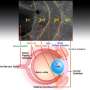
Descemet stripping involves removing a small patch of the corneal endothelium (the pumping cells that stop working in FED) attached to an underlying layer (the Descemet membrane). In patients with FED, water accumulates in the cornea, the clear front window of the eye, because of the dysfunction of the pumping cells, causing reduced vision, glare and haloes. If left untreated, the condition progresses to painful blindness.
Removal of the central dysfunctional cells enables healthier peripheral cells to migrate to the center of the cornea, where they reestablish pumping capacity and removal of fluid from the layers above. This gradually restores clear vision.
"Although Descemet stripping is a relatively simple procedure, its potential is revolutionary," Colby said. In 2015, 14,000 corneal transplants were performed in the United States, just for FED, the most common reason for this operation. The transplants work well, but the tissues are expensive and there is a limited supply in some areas of the world. Because the corneal transplant tissue is foreign, patients must apply topical steroids for the rest of their lives to dampen their immune response and prevent rejection of the transplanted cells. Steroid eye drops are known to cause glaucoma and cataract and can predispose to infection.
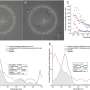
The researchers classified patients into four groups based on how they responded to Descemet stripping. Fast responders regained clear vision within a month after surgery. Responders recovered within three months. Slow responders took more than three months. Nonresponders had persistent corneal edema and required endothelial keratoplasty—a streamlined cornea transplant.
Of the 13 eyes treated, four were fast responders, four were responders and two were slow responders.
The next step is to try to understand why some patients, about one out of four, don't respond to removal of the dysfunctional cells. Fuchs dystrophy is a polygenic disease, but in the last few years researchers have found connections between the extent of a repeating nonsensical genetic abnormality seen in other neurological diseases and the severity of FED. Colby hopes to find genetic clues that predict which patients are most likely to respond to this approach.
Thorp, the first patient treated, had 20/20 vision when last assessed in January of 2016 at the University of Chicago, 24 months after his operation. He was first diagnosed with FED and had a cornea transplant in his right eye in 2002, a two-stage operation. It was successful, but the recovery process meant "foggy vision" in that eye for nearly a year. This prevented him from driving.
That eye slowly recovered, but by 2013 vision in the left eye began to decline. After Colby offered her new procedure and explained the logic behind it, Thorp felt "a great deal of confidence and understanding in what she was doing," he said. He volunteered to go first.
"It certainly turned out to be worth it," Thorp said. His operation, removal of a cataract plus Descemet stripping, took less than 30 minutes. That was "about 20 minutes for the cataract and one minute for the stripping," he recalled.
"After I performed Mr. Thorp's surgery, I waited eight months to make sure nothing unexpected happened to his cornea," Colby said, "then I started offering the procedure to patients whom I felt could benefit."
"Few things remind you as constantly as deteriorating vision," Thorp recalled. "Your world steadily narrows as you lose the ability to see. But mine expanded again at the other end. I remember walking the dog at night right after the operation. Each night, the streetlights would be a little more in focus. You could see the improvement, night after night over the course of a few weeks, like the fog lifting out of London. It was cool. Really cool."
More information: Durga S. Borkar et al, Treatment of Fuchs Endothelial Dystrophy by Descemet Stripping Without Endothelial Keratoplasty, Cornea (2016). DOI: 10.1097/ICO.0000000000000915