Finding skin cancer in a flash
The typical nude skin cancer checks with long photo sessions at your dermatologist's office to track any suspicious skin marks just got a lot more accurate, while reducing the chance of unnecessary biopsies.
UConn Health is the only institution to date in Connecticut to offer the latest advanced smart technology that hunts for skin cancer and keeps an eye on changing moles.
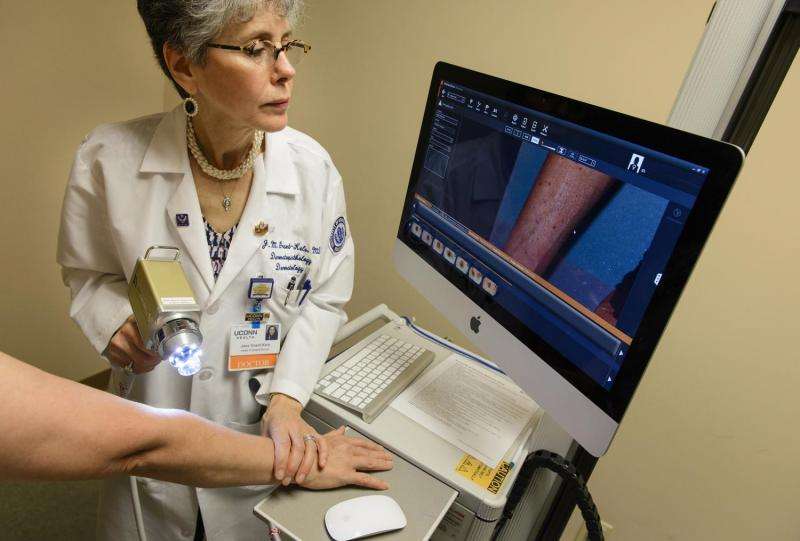
An integrated body-scanning camera and smart software technology "helps us find skin cancer in a flash," says Dr. Jane Grant-Kels, professor and vice chair of UConn Health's Department of Dermatology and director of the UConn Cutaneous Oncology Center and Melanoma Program.
The technology, called FotoFinder Bodystudio Automated Total Body Mapping, allows dermatology staff to take 20 or more photos of a patient's entire body, including the palms and the soles of the feet, in about 10 minutes. It also allows easy comparison of photographs visit after visit, and alerts the dermatologist to changes or new growths.
"This technology is going to help us save more lives from skin cancer and melanoma," says Grant-Kels. "It allows for early detection and a more exact science of monitoring patients' skin changes."
If concerning growths are detected, another recently arrived technology called In Vivo Reflectance Confocal Microscopy uses a non-invasive optical imaging technique that provides a high-resolution cellular image of the skin. This new technology is safe and painless, and in many cases can be used in lieu of a painful skin biopsy.
"FotoFinder coupled with Confocal will help us go a long way to reducing the number of biopsies performed, including unnecessary biopsies of non-cancerous skin growths," Grant-Kels says.
For baseline and follow-up photo sessions using the FotoFinder technology, a patient will be guided by a red laser light and a specially designed floor mat to ensure proper positioning. The smart body-scanning camera automatically moves into various positions to take photos of the entire body, and the software module rapidly stitches the photos together for the dermatologist to review.
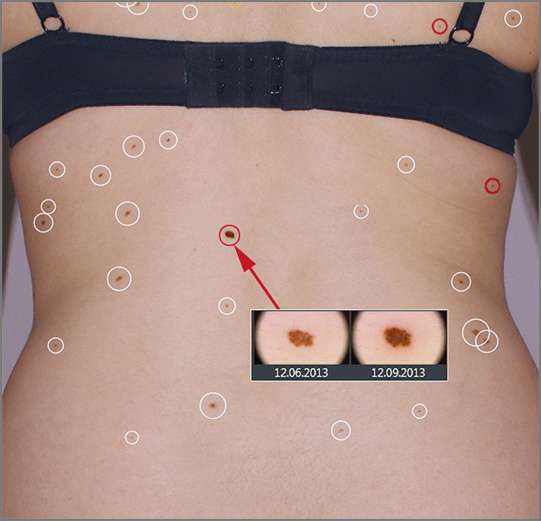
After the patient's follow-up photo session, within seconds the system uses its computer technology to precisely place the most recent skin images atop the baseline photos. The software seamlessly aligns and analyzes the new and old photos, and then circles all the detected new and visibly changed skin lesions and moles.
White circles around lesions or moles signal to the dermatologist no change; yellow circles signal caution to the doctor, as the lesion or mole has changed since the last visit; and red circles raise alarm for the doctor, as a new lesion or mole growth has been identified. This allows the dermatologist to investigate the most alarming skin lesions first.
The technology also allows dermatologists to compare lesion or mole photos side by side and to quickly zoom from 20x- up to 70x-magnification to examine suspicious areas in high-resolution and determine which spots to examine more closely with the traditional handheld dermoscopy tool. The system also includes high-tech, handheld electronic dermoscopy with a built-in medicam for even closer examination and additional photo captures. Plus, the machine is mobile and can be moved easily among exam rooms.

Grant-Kels recommends that patients with many moles or a family history of skin cancer or melanoma see a dermatologist every six months.
"I am glad to report that UConn Health now has every new FDA-approved technology to help patients manage skin health, placing us on the cutting-edge of skin cancer prevention, detection, and treatment," she says.
If you have a lot of moles or a family history of skin cancer or melanoma, the dermatologists at UConn Health recommend you should be seeing your dermatologist every six months.



















