August 27, 2016 report
Conquering the lysosomal storage disorders with genetic engineering
(Medical Xpress)—The motivation by fear, anger, and love to preserve self, kin, and others perches near the pinnacle of our existence. Triumph in the face of a seemingly insurmountable medical adversity by the creation of some tangibly successful treatment, virtually out of thin air, invariably strings together countless moments of courage and heroism to cut a continuous path of sheer human elegance through time that is a privilege to behold. The movie 'Lorenzo's Oil', and the book 'My Brother's Keeper', are two such popular accounts of families who brought the fight and won the fight against rare neurodegenerative disorders; a third is the now unfolding story of a family fighting against a debilitating lysosomal storage diseases known as Sanfilippo Syndrome, or MPSIIIa (mucopolysaccharidosis IIIa).
Lorenzo Odone ultimately died from aspiration pneumonia acquired after accidentally getting food stuck in his throat, but that wasn't until after he was thirty. He reached that age in no small part because his parents carefully developed a unique regimen of oleic and erucic acid to counter the accumulation of long chain fatty acids in his myelin that is characteristic of adrenoleukodystrophy. Similarly, Stephen Heywood died after his respirator accidentally detached, but that wasn't until he was 37. His brother Jamie helped him reach that age in part by developing novel treatments for his ALS.
When Karen Aiach and her husband learned in 2005 that their daughter Ornella had MPSIIIa, Karen founded Lysogene www.lysogene.com/ to develop a gene therapy to treat it. Today Lysogene has already completed initial studies to replace the defective heparin N sulfatase enzyme in MPSIIIa and is about to enter the next phase of their clinical trials to demonstrate its ability to halt disease progression. Lysogene recently presented their gene therapy at the 14th International Symposium on MPS last month in Germany.
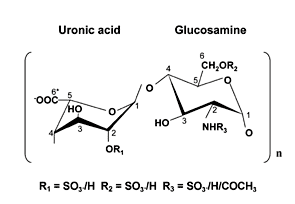
The defective MPSIIa enzyme is encoded by the N-sulphoglucosamine sulphohydrolase gene on chromosome17. It is one of four separate enzymes (the others are responsible for MPSIIIb,c,&d) that sequentially break down heparin sulphate. There is also potential to treat thiskind of disease from the supply side, namely by trying to reduce the amount of heparin sulfate hanging around by interfering directly with the synthesis or elongation of the polymer. For example, efforts to use siRNA to target the heparin synthesis genes EXTL2 and EXTL3 are already being explored elsewhere.
(The movie is available at www.freethinkmedia.com/shows/s … ise-of-gene-therapy/ )
Despite now having a fairly large amount of genetic, biochemical, and even anecdotal information about this class of rare orphan diseases, we still have very little actual understanding or knowledge of how to treat them. We can imagine a way of towing ourselves out of this unfortunate quagmire by hooking on to something that has at least two important things going for it: First, it should be something that is central to every major known cellular function. In other words, a hub through which the major behavioral outputs of a cell can be connected to the major metabolic inputs. Secondly, it should be something for which we already posses a trove of powerful insight. One thing that clearly fits that bill are the cell's mitochondria.
Not being an expert in lysosomal storage disorders I found Dr. Bruno Benitez on social media and asked him a few questions, including potential links to mitochondria:
-What's new in lysosomal storage and does CRISPR technology have the potential to revolutionize gene therapies like those being developed at Lysogene?
"The lysosome has turned out to be a key factor in energy balance for cells. It is not the place of just "garbage" anymore; it is the organelle that recycles macromolecules (hydrolyses and proteinases), senses the metabolic state (mTOR) and signals the nucleus (TFEB) to either launch or prevent a massive transcriptional response to the cellular state. Thus, studying LSDs has become a more dynamic area that integrates multiple disciplines.
Lysogene has been focused on gene therapy since the beginning; they have enough experience in gene therapy that it would be very risky of them to shift focus to CRISPR now. I would say that currently our best bet is gene therapy because we have good vectors, many clinical trials are underway, and it has been approved in Europe. CRISPr has the potential to become the standard, but many experts in the field think it is too soon to move it to clinical trials. In addition, LSDs are caused by loss-of-function mutations that often include very large deletions or heterozygous compound mutations, which makes them difficult to target with CRISPR."
-Is there neurological benefit to treating the disease peripherally, ie, with treatments that can't penetrate the BBB, and therefore target peripheral issues only (for example, hepatomegaly)?
"LSDs are systemic diseases; 75% of LSDs have a neurological component, and you are right, therapies that don't target the CNS are less efficacious. But for some LSDs, the main problem lies in the periphery, and enzyme replacement provides very good benefits for those. Gene therapy is currently used directly in the CNS by intracranial or intrathecal injections. Although you can "fix" the CNS, you also have to target the systemic disease, therefore, the best strategy is a combination of therapies that target both CNS and other organs."
-Does the progressive disease etiology indicative of storage disorders hint at a potential energetic/mitochondrial component? If more than just a developmental issue is there some hope that disease could be partly reversible?
"LSDs are the primary result of lysosome dysfunction. Recently, it has been shown that the lysosome plays a key role as a nutrient sensor, and thus, is a key factor in cellular energy balance. Thus, I agree with you that LSDs have an energy imbalance. In addition, recall that mitophagy is at the end executed by the lysosome, therefore, if the lysosome is dysfunctional, the recycling of malfunctioning or aged mitochondria is also impaired.
Some LSDs have a clear developmental component, but it is not clear in many others in which the patients are born healthy but months or years after birth start to show neurological or systemic signs of the diseases. In LSDs where the substrate that accumulates is not toxic, the cellular and systemic changes are reversible once we provide the enzyme that is lacking. The key point here is that early detection and new born screening is critical to help these patients as soon as possible for those LSDs where some therapies are already available."
-That seems to be a great point, ie. that one implication of an overloaded lysosomal degradation system could be compromise of mitophagy. It doesn't seem unlikely to ever reverse physical effects like brain structural anomaly or other craniofacial variance, but if we had some clue as to the puzzling behavioral issue origins, like the anger outbursts, that would seem to go a long way too. Exactly how these seemingly frustrated biochemistries, be it lysosomal storage, or something like purine salvage in HGPRT deficiency, manifest themselves behaviorally is perhaps, I would guess, the final frontier?
"As for the evidence of alterations in mitophagy, the main component of the storage material in Batten disease (Neuronal ceroid lipofuscinoses) is the mitochondrial ATP synthase subunit c. The involvement of the mitochondria changes in LSDs has not been properly studied yet but the metabolic defects are well known.
I agree, LSDs field has been focused on therapies for a very long time (understandable) but nowadays we are starting to understand the "new" roles of the lysosome in cell physiology and in some other diseases not just LSDs.
Behavioral changes are a very complicated consequence of dysfunctional neural networks that result from dysfunctional cells, and true to be told we have no idea how they emerge. As I said earlier, early detection (exome sequencing) plus proper intervention (ERT, gene therapy, SRT, etc) will prevent rather than reverse the complications."
© 2016 Medical Xpress

















