Researchers discover new regulator in glucose metabolism
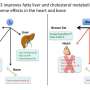
A key genetic switch in the liver regulates glucose metabolism and insulin action in other organs of the body. Researchers of Helmholtz Zentrum München, in collaboration with colleagues of the Heidelberg University Hospital, Technische Universität München and the Medical Faculty of the University of Leipzig, have now reported these findings in the journal Nature Communications.
Diabetes mellitus is a chronic disease that has become increasingly prevalent in the population: More than six million people are affected by the disease alone in Germany. It is characterized by a disruption of the glucose metabolism and (except for type 1 diabetes) an impaired response of the body to the hormone insulin. Scientists are currently seeking to find the cause and possible regulators of the disease in order to intervene therapeutically.
A team led by the metabolism expert Professor Stephan Herzig, director of the Institute for Diabetes and Cancer at Helmholtz Zentrum München (IDC), has discovered a new mechanism that is responsible for the regulation of the glucose metabolism. The transforming growth factor beta 1-stimulated clone 22 D4, abbreviated TSC22D4, acts as a molecular switch in the liver and from there regulates genes that can influence the metabolism throughout the body.
Approach from Cancer Research
"The current study is a successful continuation of our research activities with colleagues from the Internal Medicine at Heidelberg University Hospital," said study leader Herzig, who left Heidelberg in 2015 to become director of the Institute for Diabetes and Cancer at Helmholtz Zentrum München. Already in 2013 the researchers showed that increased production of TSC22D4 in the liver of mice with cancer leads to severe weight loss (cachexia) . In the present study, they investigated the role of this gene regulator in connection with diabetes.
"The strong influence of TSC22D4 on the metabolism in tumor diseases suggested that it could also play a role in metabolic diseases," said first author Dr. Bilgen Ekim Üstünel of the IDC. In the current study, the researchers showed in diabetic mice that inactivation of TSC22D4 led to an improvement of the insulin action and glucose metabolism. Further analyses revealed that TSC22D4 in particular inhibits the production of the lipocalin13 protein, which is released as a messenger substance from the liver and can regulate the glucose metabolism in other organs.
To check the relevance of the new mechanism in the clinic, the researchers examined liver tissue specimens of 66 patients with and without type 2 diabetes. They found that in the liver of the diabetes patients compared to people with normal glucose metabolism, the TSC22D4 gene was expressed significantly more often and lipocalin13 was produced correspondingly less often. "For the treatment of diabetes there is only a very limited number of therapeutic targets," said Herzig. "Next, we want to investigate whether our findings can lead to the development of a new therapeutic approach to treat diabetes and insulin resistance."
More information: Bilgen Ekim Üstünel et al. Control of diabetic hyperglycaemia and insulin resistance through TSC22D4, Nature Communications (2016). DOI: 10.1038/ncomms13267