Biomarker may predict which formerly treated cancer patients will develop highly fatal form of leukemia
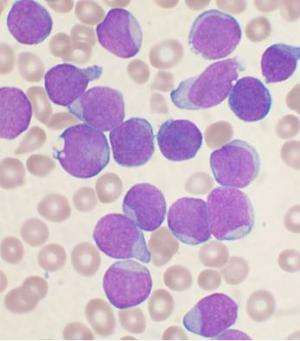
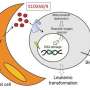
Patients successfully treated for breast, colon and other cancers can go on to develop an often-fatal form of leukemia, sometimes years after completion of treatment, due to a genetic mutation leading to secondary malignancies known as therapy-related myeloid neoplasms (t-MNs).
A study conducted by researchers at The University of Texas MD Anderson Cancer Center revealed pre-leukemic mutations, called clonal hematopoiesis, may predict whether patients develop t-MNs. Clonal hematopoiesis appears to function as a biomarker for patients who develop t-MNs, a leukemia recognized for its extremely poor prognosis. The study findings were published today in The Lancet Oncology and presented at the annual meeting of the American Society of Hematology in San Diego.
"Therapy-related myeloid neoplasms occur in about 5 percent of cancer patients who were treated with chemotherapy and/or radiation therapy," said Andy Futreal, Ph.D., chair ad interim of Genomic Medicine. "In most cases, it is fatal, and currently there is no way to predict who is at risk or prevent it."
Being able to detect t-MNs earlier is crucial given that the disease usually occurs three to eight years following chemotherapy and/or radiation therapy.
"T-MNs are a problem that needs urgent attention," said Koichi Takashi, M.D., assistant professor of Leukemia and Genomic Medicine and a co-author on the Lancet Oncology paper. "Since many cancer patients are now living longer, t-MNs are an increasing concern for many cancer survivors."
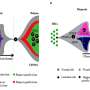
Futreal's team studied 14 patients with t-MNs and found traces of pre-leukemic mutations or clonal hematopoiesis in 10. To determine if pre-leukemic mutations could reliably predict whether the patients would develop leukemia, the researchers compared prevalence of pre-leukemic mutations in the 14 patients with 54 patients who did not develop t-MNs after therapy.
"We found that prevalence of pre-leukemic mutations was significantly higher in patients who developed t-MNs (71 percent) versus those who did not (26 percent)," said Futreal. "We also validated these findings in a separate cohort of patients. Based on these findings, we believe pre-leukemic mutations may function as a new biomarker that would predict t-MNs development."
In the sample of 14 patients with t-MNs, the team looked at samples of bone marrow at the time of t-MNs development and blood samples obtained at the time of their primary cancer diagnosis.
"We found genetic mutations that are present in t-MNs leukemia samples actually could be found in blood samples obtained at the time of their original cancer diagnosis," said Takahashi. "Based on this finding, we believe the data suggest potential approaches of screening for clonal hematopoiesis in cancer patients that may identify patients at risk of developing t-MNs, although further studies are needed."