Bone marrow inflammation predicts leukemia risk
Cancer is generally thought to arise from genetic damage within individual cells, but recent evidence has suggested that abnormal signaling in the surrounding tissue also plays an important role. In a study published September 22 in Cell Stem Cell, researchers show that inflammatory signaling in the bone marrow tumor environment is a key driver of malignancy and predicts the development of leukemia in mice and humans.
"This discovery sheds new light on the longstanding association between inflammation and cancer," says senior study author Marc Raaijmakers of the Erasmus MC Cancer Institute. "The elucidation of the molecular mechanism underlying this concept opens the prospect of improved diagnosis of patients at increased risk for the development of leukemia and the potential of future, niche-targeted therapy to delay or prevent the development of leukemia."
Leukemia is a type of cancer in which hematopoietic, or blood-forming, stem cells in the bone marrow give rise to a large number of abnormal white blood cells. But in addition to hematopoietic stem cells, the bone marrow contains mesenchymal stem cells, which generate bone, cartilage, muscle, and fat cells that support the formation of blood and fibrous connective tissue. In a recent study, Raaijmakers and his team discovered that genetic mutations in mesenchymal stem cells located in the bone marrow tumor environment can induce malignant changes in hematopoietic stem cells, increasing the risk of leukemia in mice. However, the molecular mechanisms by which the tumor microenvironment contributes to the development of cancer remained unclear.
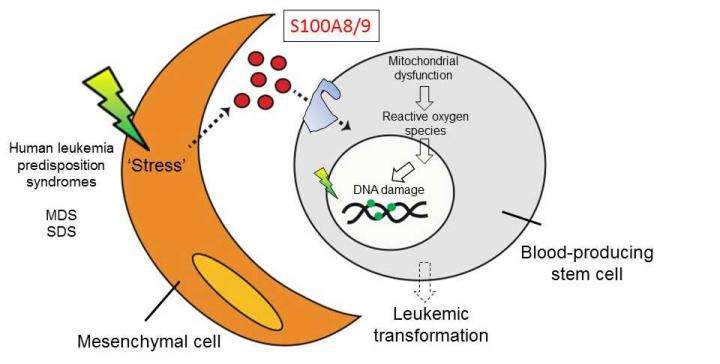
To address this question, Raaijmakers and his collaborators used massive parallel RNA sequencing of mesenchymal cells in mice with the pre-leukemic disorder Shwachman-Diamond syndrome (SDS) and bone marrow samples from patients with a range of pre-leukemic syndromes, including SDS and myelodysplastic syndrome (MDS). This analysis revealed that mesenchymal cells in these disorders are under stress, leading to the release of inflammatory molecules called S100A8 and S100A9, which cause mitochondrial and DNA damage in hematopoietic stem and progenitor cells. Moreover, activation of this inflammatory pathway in mesenchymal cells predicted the development of leukemia and clinical outcomes in human patients.
If confirmed in a larger cohort of patients, the findings could lead to the development of diagnostic tests, such as staining bone marrow biopsies or imaging studies, to identify patients at risk of developing leukemia. "These high-risk patients could be treated more aggressively at an earlier stage, thereby preventing or slowing down disease progression," Raaijmakers says. "Moreover, the findings suggest that new drugs targeting the inflammatory pathway should be tested in future preclinical studies."
More information: Noemi A. Zambetti et al, Mesenchymal Inflammation Drives Genotoxic Stress in Hematopoietic Stem Cells and Predicts Disease Evolution in Human Pre-leukemia, Cell Stem Cell (2016). DOI: 10.1016/j.stem.2016.08.021