January 26, 2017 report
Two leukemia babies in remission after injection of new kind of edited T-cells
(Medical Xpress)—Two babies given an experimental kind of edited T-cells to treat their leukemia remain in remission after more than a year, doctors working on the case report in a paper published in the journal Science Translational Medicine. The research team is affiliated with several institutions in the U.K.
The cells used to treat the two babies were part of a modified form of CAR-T cell therapy, in which a virus is used to edit a gene in an immune cell taken from the patient to cause it to attack cancer cells—once ready, it is injected back into the patient. This approach has been found to be quite successful in a number of children, but is not nearly as applicable to sick infants with low numbers of healthy immune cells. In this new effort, the researchers started with immune cells from a donor and then modified them in several important ways.
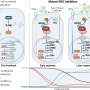
The first change was to disable the gene responsible for causing the immune system to attack the donated cell after recognizing it as a foreign body. Another change caused the edited cells to recognize and attack cancer cells. A third change was part of an effort to offset the likelihood of the recipient developing graft-versus-host disease.
The first recipient of the experimental cells was an 11-month-old girl who received her edited cells in June of 2015—she was followed by a 16-month-old child who was injected in December of 2015. Both of the girls also underwent chemotherapy. They also received bone marrow transplants after a period of time to restore their immune systems and to flush the edited cells from their bodies. One of the babies developed graft-host disease despite the gene change, which was promptly resolved with treatment. Both girls are now home with their families and are reportedly in good health.
The treatment was experimental, which means it has not been approved for use by governmental agencies—it was only allowed in this case because all other options had been exhausted. Trials of various forms of CAR-T cell therapy are ongoing, some of which have shown great promise, suggesting that some may be approved soon.
More information: Waseem Qasim et al. Molecular remission of infant B-ALL after infusion of universal TALEN gene-edited CAR T cells, Science Translational Medicine (2017). DOI: 10.1126/scitranslmed.aaj2013
Abstract
Autologous T cells engineered to express chimeric antigen receptor against the B cell antigen CD19 (CAR19) are achieving marked leukemic remissions in early-phase trials but can be difficult to manufacture, especially in infants or heavily treated patients. We generated universal CAR19 (UCART19) T cells by lentiviral transduction of non–human leukocyte antigen–matched donor cells and simultaneous transcription activator-like effector nuclease (TALEN)–mediated gene editing of T cell receptor α chain and CD52 gene loci. Two infants with relapsed refractory CD19+ B cell acute lymphoblastic leukemia received lymphodepleting chemotherapy and anti-CD52 serotherapy, followed by a single-dose infusion of UCART19 cells. Molecular remissions were achieved within 28 days in both infants, and UCART19 cells persisted until conditioning ahead of successful allogeneic stem cell transplantation. This bridge-to-transplantation strategy demonstrates the therapeutic potential of gene-editing technology.
© 2017 Medical Xpress