Connection between renal failure and 'bad' mitochondria described
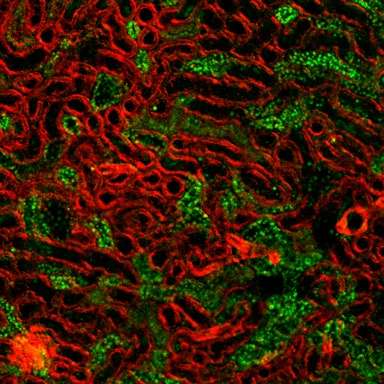
Biologists of the Lomonosov Moscow State University have suggested an approach to prevent kidney injury after ischemia. Moreover, the scientists explain why these mechanisms become non-protective in aging kidneys. The results of the study are published in Scientific Reports.
The project is focused on elucidation of mechanisms underlying such severe pathologies as renal failure caused by ischemia (blocking of blood supply). Biologist Egor Plotnikov, one of the corresponding authors of the article, says, "We've shown that it's possible to prevent kidney damage by its preliminary 'training' by short periods of ischemia. However, our main discovery is the fact that this mechanism is disabled in older animals and, as a result, a kidney becomes unprotected. It is an extremely important problem, as the major part of clinical cases of renal failure occurs in aged patients. To afford the protection of their kidneys would be a great success for medicine."
The experiments included young rats and a strain of prematurely aged rats. Egor Plotnikov says, "In the current article, we describe what underlies such a loss of adaptation in kidney in old rats (and, probably, in old people). All cells have a mechanism of 'quality control,' which provides removal of damaged cellular elements (in our case—damaged mitochondria) responsible for permanent self-renewal of the system. However, these mechanisms become broken in old kidneys and its adaptive mechanisms stop functioning."
The basic mitochondrial function in any cell is energy production. Due to oxidation of substrates, energy is stored in the form of a universal energy form, ATP (adenosine triphosphate). A mitochondrion operates as a power station, as energy is initially stored in the inner mitochondrial membrane in the form of electrical potential, and only later is it converted into ATP. Additionally, mitochondria have many other functions—synthesis of some hormones and other substances, detoxification, and other functions including determination of cell fate—to die or to survive. Moreover, most of these functions are more or less functionally connected with the very electrical transmembrane potential.
The scientists revealed that a considerable number of mitochondria in old rats have lower transmembrane potential, and this process inevitably leads to cell death. Since kidney cells cannot proliferate, they are irreplaceable, and as more die, it is harder for the organism to recover from renal injury. When this happens, a kidney is no longer able to fulfill its main function: removing products of metabolism, many of which are quite toxic. That's why such "bad" mitochondria should be removed.
In a young kidney, this quality control function depends on the transmembrane potential of mitochondria—when it drops below the critical value for a long period, a mitochondrion gets a "black label" in the form of a special protein—PINK-1. Such a labeled mitochondrion undergoes a process of self-destruction (autophagy) and becomes destroyed in a lysosome (a special organelle acting as a cellular "stomach"). In cells of old kidneys, this process is broken, and damaged mitochondria with low potential cannot be destroyed; instead, they increase in number.
The scientists say it is possible they discovered a factor that functions as a marker of old (or possibly prematurely old) cells. This factor is protein acetylation. In an organ damaged by ischemia, the number of proteins to which the acetyl group (an acetic acid moiety) is attached significantly increases. But most importantly, the number of acetylated proteins in a kidney rises with age.
Egor Plotnikov says, "We've shown that training (preconditioning) doesn't work in old age because bad mitochondria aren't removed by autophagy. There is the following process: We block the blood supply of the kidney, depriving it of oxygen and substrates, and under these conditions, the weakest mitochondria in the cells lose their potential and are immediately removed by the quality control system. As a result, the purges of the mitochondrion population take place, and only the healthy ones survive. That's why, in the case of severe kidney ischemia, mitochondria can cope with the damage and they survive. And what happens in old rats? We do kidney preconditioning, mitochondria lose their potential, but they aren't removed, as the clean-up system operates poorly. As a result of such training, bad mitochondria accumulate in an old cell, and in case of kidney ischemia, everything gets even worse."
It has been previously demonstrated by another scientific group that the mechanism of ischemic or hypoxic training also operates in humans. Moreover, clinical practice shows that organs of aged people don't respond to many defensive agents (namely, drugs, simulating preconditioning). As it's quite difficult to cut off the blood supply in some organs in a human body without surgical interventions, so-called remote preconditioning (distant training) is used in clinics. This technique interrupts the blood supply of an organ (for instance, a muscle) using a blood pressure cuff, during which an arm or a leg of a patient is squeezed for several minutes. This procedure has not been applied for kidney protection yet, but positive cardiac effects have been observed. However, these techniques are less effective in old patients.
Egor Plotnikov concludes: "This project opens a prospect for renal failure treatment. Moreover, mechanisms that we discovered are quite universal, so it's obvious that they are also applicable not only to kidney ischemia, but also to other renal pathologies. It's becoming clear why aged people suffer from severe kidney injury so often and why most modern treatment methods are ineffective for old people. Our data suggest the need for further development of drugs, which could help an old kidney to recover capacity to resist ischemia and increase its adaptation reserves."