June 30, 2017 report
Lack of a hormone in pregnant mice linked to preeclampsia
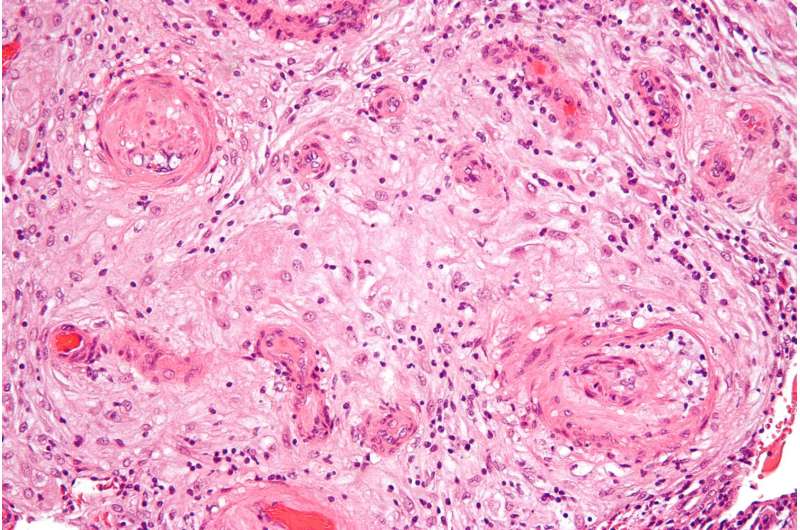
(Medical Xpress)—A team of researchers from Singapore, the Netherlands and Turkey has isolated a hormone in pregnant mice that appears to be associated with preeclampsia—a pregnancy-related condition characterized by high blood pressure and kidney problems. In their paper published in the journal Science, the team describes how they studied the hormone elabela in pregnant mice and their hope that their findings may lead to a treatment for preeclampsia in humans.
Preeclampsia is a very serious ailment for pregnant women—their blood pressure rises quickly and dramatically and they experience buildup of a protein in their urine. Fortunately, the condition is not very common, occurring in just 5 to 8 percent of all pregnancies. But if not treated quickly, it can be fatal. In this new effort, the researchers report that they were studying the hormone elabela to learn more about what it does in both mammals and fish. They found that the hormone was typically present in the placenta and in the bloodstreams of pregnant mice.
After wondering what might happen if the hormone were absent during pregnancy, they genetically altered some test mice and then observed what happened as they became pregnant. They report that the absence of the hormone resulted in vascular abnormalities in developing embryos and in placentas—both symptoms common with preeclampsia. That prompted the team to take a closer look at what was occurring—RNA analysis of placentas that lacked the hormone showed gene expression profiles that suggested hypoxia conditions, which included expressions, prior research has shown, that are part of the blood vessel building process—another symptom common in women with preeclampsia. The group also tested the genetically altered pregnant mice and found that they had abnormal levels of protein in their urine and heightened blood pressure levels. Additionally, their pups were underweight—all symptoms of preeclampsia.
Excited by their findings, the team injected the hormone, replacing what had been lost, into the impacted test mice and found that their preeclampsia symptoms disappeared almost immediately. It is not clear if the same hormone, or lack of it, might play a role in preeclampsia in humans, but the team hopes to find out. If the work is transferable, it might finally provide a means for spotting a tendency toward preeclampsia for pregnant women, and possibly warding off the condition altogether.
More information: Lena Ho et al. ELABELA deficiency promotes preeclampsia and cardiovascular malformations in mice, Science (2017). DOI: 10.1126/science.aam6607
Abstract
Pre-eclampsia (PE) is a gestational hypertensive syndrome affecting between 5 and 8% of all pregnancies. While PE is the leading cause of fetal and maternal morbidity/mortality, its molecular etiology is still unclear. Here, we show that ELABELA (ELA), an endogenous ligand of the apelin receptor (APLNR, or APJ), is a circulating hormone secreted by the placenta. Elabela but not Apelin knockout pregnant mice exhibit PE-like symptoms, including proteinuria and elevated blood pressure due to defective placental angiogenesis. In mice, infusion of exogenous ELA normalizes hypertension, proteinuria, and birth weight. ELA, which is abundant in human placentas, increases the invasiveness of trophoblast-like cells, suggesting that it enhances placental development to prevent PE. The ELA-APLNR signaling axis may offer a new paradigm for the treatment of common pregnancy-related complications, including PE.
© 2017 Medical Xpress