A new mutation in kidney disease
Medullary cystic kidney disease type 1 (MCKD1) is a rare genetic kidney disease. Despite this, because it is an autosomal dominant disease, once the mutation is in a family, many family members are affected. Current diagnostic methods discover the disease late in its development. Osaka University researchers studied one family in which 9 of 26 members were positive for MCKD1 and found a new mutation in the MUC1 gene that may act as an early marker of the disease.
"Besides renal failure and genetic testing, there is little we have to identify the disease," says Associate Professor Jun-Ya Kaimori, a nephrologist at Osaka University Hospital. "There are very few early signs that show illness."
At the point of renal failure, patients are usually left with only extreme and invasive treatment options, such as dialysis or transplantation.
"MCKD1 is caused by a single mutation in MUC1 gene discovered in 2013," he continued.
The mutation is located in a region of the gene that includes GC-rich variable number of tandem repeats (VNTR). This, explains Kaimori, makes it very difficult to analyze.
"The standard technique to analyze is next-generation sequencing. VNTR have a tertiary structure that makes it very difficult to analyze by next-generation sequencing. Even finding the mutation took immense time and effort," he said.
In his latest research study, Kaimori and his colleagues used whole-exome sequencing to analyze the gene and found a second mutation outside the VNTR.
"The mutation was a deletion of just two base pairs, but that was enough to change the protein structure."
The original MUC1 mutation was found by a collaboration of scientists from U.S. and European institutes. When asked why his group found the mutation but the international collaboration did not, Kaimori frankly replied, "It was an unexpected discovery."
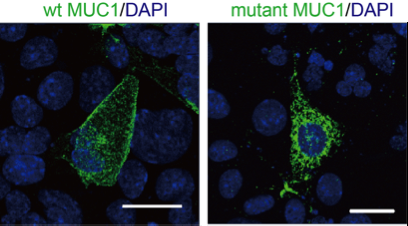
Unlike the first mutation, the location of the new mutation allowed the scientists to study the effects of the mutated protein further. Experiments suggested that the mutation disrupts the function of MUC1 and changes its location inside cells. This last observation excited Kaimori, because it suggested a potential biomarker to diagnose patients before renal failure.
"We found patients had high levels of mutant MUC1 in urinary exosomes, but healthy people had normal MUC1 in urinary exosomes. These results suggest we can use urinary exosomes for non-genetic testing to evaluate the risk of MCKD1."
More information: Satoko Yamamoto et al. Analysis of an ADTKD family with a novel frameshift mutation in MUC1 reveals characteristic features of mutant MUC1 protein, Nephrology Dialysis Transplantation (2017). DOI: 10.1093/ndt/gfx083