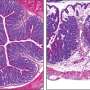
Antibiotics taken late in pregnancy can increase risk for IBD in offspring

A study by researchers at the University of Chicago Medicine shows that when mice that are genetically susceptible to developing inflammatory bowel disease (IBD) were given antibiotics during late pregnancy and the early nursing period, their offspring were more likely to develop an inflammatory condition of the colon that resembles human IBD.
The antibiotic treatment also caused lasting changes in the gut microbiome of mothers that were passed on to their offspring. While their offspring developed disease, adult mice given antibiotics did not see an increase in IBD. This suggests that the timing of antibiotic exposure is crucial, especially during the early developmental period after birth when the immune system is undergoing maturation.
"The newborn mice inherited a very altered, skewed population of microbes," said Eugene B. Chang, MD, Martin Boyer Professor of Medicine at the University of Chicago, Director of the Microbiome Medicine Program of the Microbiome Center, and senior author of the study, published this week in the journal Cell Reports. "None of the mothers developed IBD, but even though they had the same genetic background, the offspring with an altered microbiome during this critical period of immune development became highly susceptible to the development of colitis."
Chang cautioned, however, that these results from an animal study should not be taken as a reason for pregnant women or those nursing newborn infants to avoid antibiotics when they are needed to treat dangerous bacterial infections. Instead, he said, it should serve as a reminder that best practices dictate avoiding casual, indiscriminant over usage 'just to be safe', say, for a common cold that is most likely caused by a virus.
"Antibiotics should absolutely be used judiciously when they're indicated," Chang said. "But we as physicians should keep in mind the importance of antimicrobial stewardship, because this study suggests that it may have long term consequences that potentially impact health and risk for certain diseases."
Lasting changes in the gut microbiome
Several epidemiological studies have suggested that exposure to antibiotics during the peripartum period (late pregnancy and the nursing period after birth) increases the risk for IBD in humans. Direct evidence for this association has been lacking, however, because of vast differences in individual gut microbiomes, challenges in controlling for variables, and the limits of conducting clinical experiments in pregnant women and infants.
To address these issues, Jun Miyoshi, MD, PhD, a postdoctoral scholar, and Alexandria Bobe, a graduate student in Chang's lab, designed a series of experiments with a standard genetic mouse model for IBD to study the timing of antibiotic treatment during the peripartum period and its impact on gut microbes and immune system development in offspring. The researchers gave cefoperazone, a commonly-used antibiotic, to mouse mothers in the late stages of pregnancy through the period that they nursed their pups, i.e. to mimic a common clinical scenario of early antibiotic exposure in humans. None of the adult mice treated with antibiotics developed colitis, but their pups exhibited a high risk for developing colitis compared to those from mothers that were not treated with antibiotics.
Using state-of-the-art, high-throughput sequencing technologies, the team also analyzed the gut microbial population structures of mothers and their offspring. The mothers showed a decrease in diversity of bacteria, and changes in the relative numbers of certain groups of bacteria. For example, there were fewer populations of Bacteroidetes and more from the phyla Firmicutes and Verrucomicrobia. Surprisingly, these changes persisted even four to eight weeks after stopping the antibiotic treatment.
The mouse pups also had similar changes in their gut bacteria, with microbial communities matching their mothers at birth. The diversity of microbes in these pups was significantly different from that of mice not treated with antibiotics, and these differences lasted into adulthood.
"What this should tell us is, at least as physicians, is that antibiotics are not as innocuous as we think they are, and injudicious, casual use of them can have consequences," Chang said. "When they're used during pregnancy or early childhood, they can disturb the development of a normal gut microbiome which would otherwise be essential for proper immune development. In genetically susceptible hosts, the inability to develop the immune system properly can have negative consequences like inflammatory bowel disease or any other kinds of complex immune disorders."
Working toward a definition of health
Chang said that understanding more about the microbiome in an unhealthy state can help scientists begin to learn how to promote the development of a microbiome that sets the stage for a healthy immune system.
"What this study showed is what an 'unhealthy' microbiome looks like, so presumably whatever is missing may be important to promote health," he said. "What we want to eventually develop is a microbial cocktail we can give to infants that ensures that they develop properly, metabolically and immunologically. That's going to have a significant impact on human health, by reducing risk for many types of diseases and by promoting wellness."
More information: "Peripartum Exposure to Antibiotics Promotes Persistent Gut Dysbiosis, Immune Imbalance, and Colitis in Genetically Prone Offspring," Cell Reports (2017). DOI: 10.1016/j.celrep.2017.06.060