Cause of spontaneous hives pinpointed by clinical study

Melbourne researchers have solved a longstanding mystery about why some people develop recurring, itchy hives without an apparent allergic trigger, a condition known as chronic spontaneous urticaria (CSU).
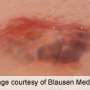
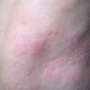
Hives or 'urticaria' are itchy raised welts on the skin caused by an inflammatory reaction. A team of researchers at the Walter and Eliza Hall Institute and the Royal Melbourne Hospital have discovered how CSU develops, and are now working towards better treatments – or even a cure – for this condition.
Dr Priscilla Auyeung, a clinical immunologist at the Royal Melbourne Hospital and clinician-scientist at the Walter and Eliza Hall Institute, said people with CSU found it very frustrating that there was no obvious trigger for their hives.
"One in five Australians will experience hives at some stage of their lives. Sometimes it's an allergy, when a reaction is linked to an external trigger or allergen – such as contact with a particular type of animal or plant, or eating a certain food," Dr Auyeung said.
"However, CSU is different. People with CSU develop recurring hives for periods of at least six weeks – and often for many years – but with no apparent trigger. Our patients often think that they're allergic to their washing powder, soap or shampoo, and sometimes even wonder if it is all in their mind."

In research published in the Journal of Allergy and Clinical Immunology, Dr Auyeung and colleagues Professor Len Harrison, Dr Diana Mittag and Professor Phil Hodgkin used samples from CSU patients attending the Royal Melbourne Hospital to investigate whether the hives were caused by immune T cells.
"We found that in the majority of people with CSU, T cells reacted to a specific protein found on other immune cells, called mast cells, in the skin. This aberrant 'autoimmune' T cell response drives the inflammation that causes itchy hives in CSU," Dr Auyeung said.
Dr Auyeung has recently begun new studies to investigate whether the autoimmune T cells that trigger CSU could be switched off by new, targeted treatments.
"We're using blood samples from CSU patients at the Royal Melbourne Hospital to home in on the precise molecules that trigger the immune response," she said.
"In recent years we've seen new 'immune modulatory' therapies developed that switch off the damaging immune response underlying other immune disorders, such as allergies and type 1 diabetes. We're hoping to use the same techniques to develop a new therapy that could potentially bring relief to people with CSU."
More information: Priscilla Auyeung et al. Autoreactive T cells in chronic spontaneous urticaria target the IgE Fc receptor Iα subunit, Journal of Allergy and Clinical Immunology (2016). DOI: 10.1016/j.jaci.2016.04.036