International eye cancer research project to improve future therapies
A new international research project, involving the University of Liverpool's leading eye cancer research group, has identified specific subtypes of ocular melanoma that will help develop improved management strategies and therapies in the future.
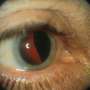
Uveal melanoma (UM) is a cancer that arises from the pigment cells (melanocytes) in the middle layer of the eye. UM are rare cancers, being diagnosed in about 600 patients in the UK each year, and differ in many ways to skin melanomas.
Although treatment of the eye for UM is usually successful through radiotherapy or surgery, up to 50% of UM patients develop metastatic disease, typically in the liver, for which there are currently no effective therapies.
In a comprehensive analysis of 80 primary UM, researchers of The Cancer Genome Atlas (TCGA) Research UM group identified and characterised four distinct subtypes that have unique genomic abnormalities, gene expression features, and patient outcomes.
This TCGA study, published in Cancer Cell this month, suggests that the four UM subtypes uncovered, each with unique molecular pathway changes and associated clinical prognoses, may require different management strategies.
The researchers deployed a range of sequencing technologies and novel analytical approaches to characterize molecularly and clinically distinct subtypes of UM. They were able to identify new and complex alterations of particular genes that otherwise would not have been found. These genomic alterations can help distinguish subtypes of UM, which carry more and less favourable prognoses, respectively.
Professor Coupland, who leads the University's Liverpool Ocular Oncology Research Group and who is Director of the North West Cancer Research Centre, made a major contribution to the TCGA UM study. LOORG contributed 25% of the intensively investigated UM samples, which came from several other international centres. The TCGA stringency criteria for the quality of examined samples with all of the associated clinical data were very high. These criteria were met by LOORG's samples, which were kept in the unique Liverpool Ocular Oncology Biobank, run by LOORG's Senior Postdoctoral scientist, Dr Kalirai. LOORG was also integral in the histomorphological evaluation of all 80 UM samples, the complex data interpretation and manuscript writing of the TCGA UM study, which ran over 3 years from start to end.
Of the research Professor Coupland said: "We already stratify UM patients into those of high- and low-risk with respect to developing metastases. The TCGA subtypes will help us refine our prognostication model, which has been successfully used in the NHS for years at the Liverpool Ocular Oncology Referral Centre and other places across the globe.
"Overall, this study expanded our basic understanding of a rare, deadly disease and revealed novel characteristics of the primary tumour that may guide the development and application of 'personalised' clinical strategies for UM subtypes in the future. We are also involved in the UMCure2020 project, which is assessing many similar aspects of UM metastases in the liver. Through the TCGA and UMCure2020 I am confident that we will make breakthroughs in the treatment of this devastating disease, as has been done in other cancers recently. We are infinitely grateful to all UM patients who allow us to use their tumour samples for this research".
More information: A. Gordon Robertson et al, Integrative Analysis Identifies Four Molecular and Clinical Subsets in Uveal Melanoma, Cancer Cell (2017). DOI: 10.1016/j.ccell.2017.07.003
mpcetoolsforhealth.liverpool.a … soap/lumpo3cr_v5.htm