Study identifies blood vessel as a therapeutic target for diabetes
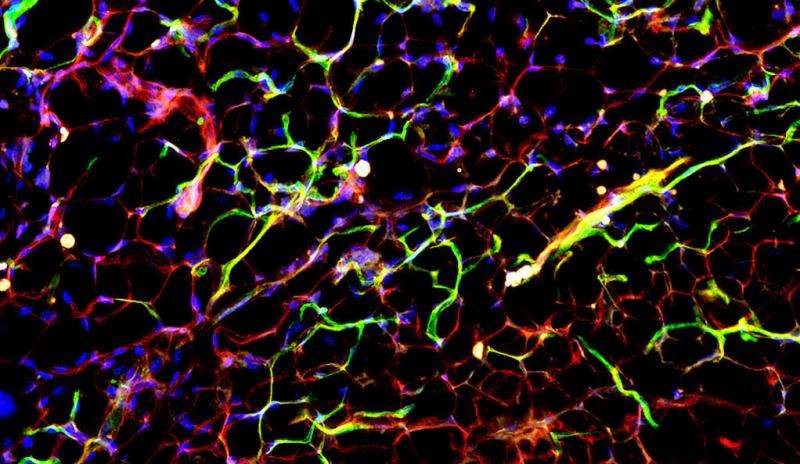
Blood vessels have an often overlooked role of regulating the transfer of nutrients from the blood to organs in the body. In a new Yale-led study, researchers have identified a role of a secreted protein, apelin, in regulating the transfer of fatty acids across the blood vessels. The study offers insights into a potential target for future therapies for type 2 diabetes.
Published in Science Translational Medicine, the study was led by cardiologist Dr. Hyung J. Chun, associate professor of internal medicine.
Researchers have long known that apelin has positive effects on the body's use of glucose and on insulin response. Yet the underlying biological mechanism was not well understood. Through experiments with mice and human samples, the research team discovered that the receptor for apelin is predominantly expressed in the endothelial cells, or the inner lining of all the blood vessels in the body. In mice lacking the receptor specifically in the endothelial cells, the researchers observed an excess of fatty acid accumulation in tissues, and complete loss of the beneficial metabolic effects of apelin. The mice also became insulin resistant, a condition that can result in increased blood sugar and type 2 diabetes.
The findings reveal how apelin and its receptor regulate the glucose-insulin balance. They also point to this pathway as a potential target for treatments to regulate metabolism and treat type 2 diabetes. Importantly, said the researchers, given previous studies describing the protective effects of apelin on atherosclerosis (clogged arteries), future development of this pathway as a therapy for diabetes may offer the added benefit of reducing the cardiovascular complications of this devastating disease.
More information: Cheol Hwangbo et al. Endothelial APLNR regulates tissue fatty acid uptake and is essential for apelin's glucose-lowering effects, Science Translational Medicine (2017). DOI: 10.1126/scitranslmed.aad4000