Cell surface protein may offer big target in treating high-risk childhood cancers
Oncology researchers studying high-risk children's cancers have identified a protein that offers a likely target for immunotherapy—harnessing the immune system in medical treatments. In cell cultures and animal models, a potent drug attached to an antibody selectively zeroes in on cancer cells without harming healthy cells.
"We have built a strong foundation for developing a completely new and hopefully much less toxic treatment for neuroblastoma, the most common cancer in infants," said study supervisor John M. Maris, MD, a pediatric oncologist at Children's Hospital of Philadelphia (CHOP). "Furthermore, our findings may also lend support to the development of other immune-based therapies, such as CAR T-cells, in children with multiple aggressive cancers in addition to neuroblastoma."
Maris, along with study leader and first author Kristopher R. Bosse, MD, and colleagues published their study today in Cancer Cell, which featured their findings as the cover story.
Neuroblastoma is a cancer of the developing peripheral nervous system that usually occurs as a solid tumor in a child's chest or abdomen, and is the most common cancer in infants. It accounts for a disproportionate share of cancer deaths in children. Over decades, CHOP clinicians and researchers have built one of the world's leading programs in neuroblastoma.
The study team used sophisticated sequencing tools to first discover molecules that are much more commonly found on the surface of neuroblastoma cells than on normal cells. "Our rationale was to identify a cell-surface molecule that an immune-based therapy could target without damaging healthy tissues," said Bosse. "Using this approach, we identified a protein called glypican-2, or GPC2." GPC2 is one of a family of glypicans—cell-surface proteins that interact with growth factors and cell surface receptors, influencing many intracellular signaling pathways important in development and cancer.
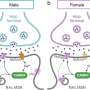
In addition to GPC2's presence on neuroblastoma cells, the study team also found that GPC2 is necessary for a neuroblastoma tumor to proliferate. Both of those facts implied that a compound that acted against GPC2 might kill cancer cells, spare healthy cells, and limit the possibility of these tumors developing "immune escape" mechanisms, in which cancer cells resist an immunotherapy by shedding the target. "Given GPC2's critical role in the growth of neuroblastomas, we hope that tumors will not be able to simply downregulate this protein in order to escape recognition by our immunotherapies that target GPC2," said Bosse.
After pinpointing GPC2 as a very promising target for therapy, the researchers next worked with their colleagues at the National Cancer Institute to search for a weapon. They developed an antibody-drug conjugate (ADC) called D3-GPC2-PBD, which combined a very specific antibody that recognizes GPC2 with a potent chemotherapy drug that is internalized specifically by cancer cells. The drug payload damages DNA in tumors, while sparing healthy tissues from its toxic effects.
In cell cultures and mouse models of neuroblastoma, the ADC robustly killed neuroblastoma cells with no discernible toxicity to normal cells. "These findings establish that this type of immunotherapy could be potentially safe and effective against neuroblastoma," said Maris. "Our next steps will be to further evaluate this ADC and also develop other immune-based therapies directed against GPC2. Because other glypicans in addition to GPC2 are overexpressed in other childhood cancers, it may also be possible to apply this approach across various types of high-risk pediatric cancers."
More information: Kristopher R. Bosse, et al, "Identification of GPC2 as an oncoprotein and candidate immunotherapeutic target in high-risk neuroblastoma," Cancer Cell, online Sep. 11, 2017.