Happy patients, healthy lungs

Diseases like chronic obstructive pulmonary disease (COPD) and cystic fibrosis (CF) are hard to treat. Lung transplant is important option for people who do not benefit from other treatments, and understanding the outcomes for these patients is crucial.
Patrick Smith, PhD, a clinical psychologist at Duke Hospital, shared his research into predictors for outcomes of lung transplant with a group of transplant physicians and surgeons at the Duke Hospital on Sept. 14.
"Patients receive transplants to live longer and to feel better," Smith said.
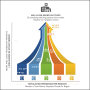
Focus on the first goal has increased the median survival time after a lung transplant to six years. But Smith began his research because of an interest in the second goal.
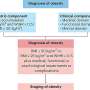
An incredibly complex, long, and difficult procedure, transplants require extensive testing and therapies before a patient enters the operating room (OR). Among the pre-operative testing is a mental health assessment to determine if any psychological issues exist that could make recovery more difficult. Mental health issues can affect adherence, or a patient's commitment to continuing the prescribed post-op medication after release from the hospital.
Smith's research found that some of these tests can be incredibly useful at predicting outcomes not previously explored; patients who show cognitive impairments before surgery were found to be more likely to fall victim to delirium, a post-operative state of confusion and psychosis that has been linked to an increased risk of complications and death.
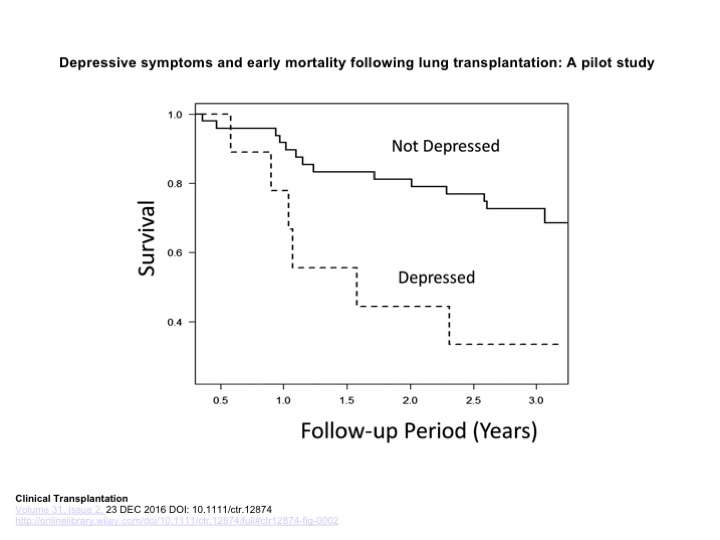
While acknowledging the usefulness of pre-operative testing, Smith also pointed out the inadequacy of this model. Failing to continue psychological assessments after the surgery and throughout the recovery means that doctors are missing important clues that could indicate how well patients will recover.
Through his research, Smith has found that the presence of depressive symptoms after transplant is actually a much more useful and accurate tool for predicting risk of mortality than symptoms exhibited before surgery.
This point is strengthened by a previous study that found that successful treatment of depressive symptoms in liver transplant patients reduced the mortality rate of depressive patients to that of their non-depressive counterparts.
These results are promising for the possibility of improving transplant outcomes; by valuing and treating both pre-operative and post-operative signs of risk, doctors can improve the outcomes for their patients and ensure the limited supply of organs is being used in the best and most successful way possible.