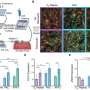
Hospital mortality rates after heart attack differ by age
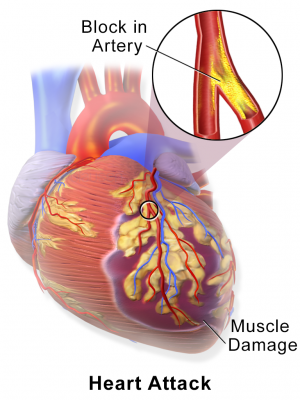
Outcomes for older patients hospitalized for a heart attack are often used as a measure of hospital quality for all patients. But a study led by Yale researchers shows that hospital mortality rates for older patients with heart attack are not necessarily representative of mortality rates for younger adults.
The findings, published in Annals of Internal Medicine, point to the need for including younger patients in assessments of hospital quality, as well as further investigation of the age-related differences, said the researchers.
The research team analyzed data for older and younger adults hospitalized for heart attack between 2010 and 2014. They calculated mortality rates within 30 days of admission and ranked hospitals based on those rates for the different age groups and for all patients with heart attacks.
The researchers found, notably, that half of the hospitalized heart attack patients were under age 65. They also observed differences in hospital 30-day mortality rates for patients under 65 compared to those over 65.
The findings shed light on an inconsistency in hospital quality for older and younger adults who suffer heart attack, the researchers said. "The assumption that the outcomes of younger patients parallel those of older patients within a hospital does not hold up," said Jeptha Curtis, M.D., associate professor of medicine and co-author of the paper.
While data on older patients, derived from Medicare records, is still valuable, said the researchers, it may not provide a complete picture of hospital quality. "We can't assume signals of quality for older adults are generalizable. We need to understand hospital quality for younger adults as well," said Kumar Dharmarajan, M.D., assistant professor of medicine and lead author.
While there are obstacles to gathering data for younger adults, whose records are not kept in one publicly available database like Medicare, the obstacles may be worth overcoming, said Dharmarajan. "Without knowing quality for younger adults, there's no way we can understand and benchmark performance to improve outcomes moving forward," he noted.
More information: Annals of Internal Medicine (2017). annals.org/aim/article/doi/10.7326/M16-2871
Editorial: Annals of Internal Medicine (2017). annals.org/aim/article/doi/10.7326/M17-2363