Availability of robotic prostate cancer surgery could be a bigger draw for patients than quality of hospital
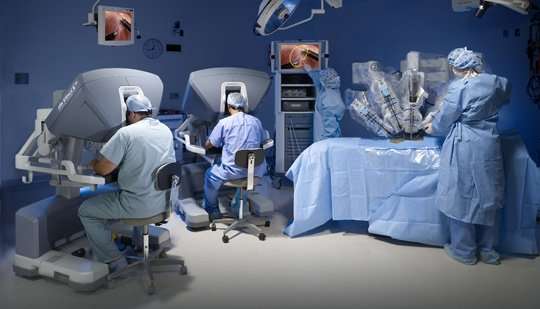
Prostate cancer patients in England may base their choice of hospital for surgery on the availability of new technology, rather than information on the quality of the hospital, according to a new study.
The reputation of a hospital or its doctors may also play a role in a patient's decision making.
The researchers behind the study say competition between hospitals has resulted in the closure of some hospitals and the adoption of robot-assisted surgery at others, even though such techniques aren't proven to improve outcomes.
The study's lead author, Dr Ajay Aggarwal from the London School of Hygiene & Tropical Medicine, said the lack of publicly available information to help judge the quality of prostate cancer surgery meant that patients have to make their choices based on other factors.
"It appears that patients use the availability of robotic prostatectomy as an indicator of high quality care, despite a lack of evidence of its superiority compared with open surgery," he said.
"NHS hospitals are subsequently investing millions of pounds into new and sometimes unproven technologies which has a direct impact on the type of care patients receive, but also the configuration of services as a whole."
The study, published in The Lancet Oncology, looked at over 19,000 men who had their prostate removed in the NHS in England between 2010-2014, and recorded where they lived and where they had surgery.
Previous work found that a third of men who had a radical prostatectomy for prostate cancer from 2010-2014 in the NHS travelled beyond or bypassed their nearest prostate cancer surgery centre, in many cases across regional boundaries.
This especially applied to younger, fitter, and more affluent men.
There were 65 centres open at the start of 2010, and 23 of these saw an increase in the number of patients compared to expected figures based on the local population. 10 of these 23 centres (43.5 percent) offered robot-assisted surgery.
More than half (37) of the 65 centres had a decrease in the number of patients, only 2 of which (5.4 percent) offered robot-assisted surgery at the start of 2010. 10 of these 37 centres closed their radical prostatectomy service. No robotic surgery centre closed during the period under study.
"NHS choice and competition policy is based on the principle that patients will travel to centres they think will provide the best service," said Aggarwal. "Closures were never intended to result from this, but the large number of patients deciding to receive treatment elsewhere meant some centres faced the risk of closures as they were no longer performing a sufficient number of procedures to sustain their service," he added.
Over the period of study the number of centres offering robot-assisted surgery more than tripled from 12 to 39.
"Even within publicly-funded systems like the NHS, competition policies have stimulated a form of centralisation through 'natural selection', as centres invest in unproven new technologies to protect their status, instead of services being regionally planned and coordinated," said Aggarwal.
"Rapid adoption of high technology therapies is not unique to prostate cancer, and further research should look at other types of cancer where new types of treatment are increasingly available as well."
Rose Gray, senior policy adviser at Cancer Research UK, said that as surgery is the cornerstone of treatment for many cancers it's vital that decisions about service planning and treatment options are based on sound evidence.
"The 2015 Cancer Strategy for England recommended that the NHS develops new ways of measuring the quality of cancer surgery," she said. "We're glad that this important work is now underway."
More information: Ajay Aggarwal et al. Effect of patient choice and hospital competition on service configuration and technology adoption within cancer surgery: a national, population-based study, The Lancet Oncology (2017). DOI: 10.1016/S1470-2045(17)30572-7