October 20, 2017 report
Evidence found of oral bacteria contributing to bowel disorders
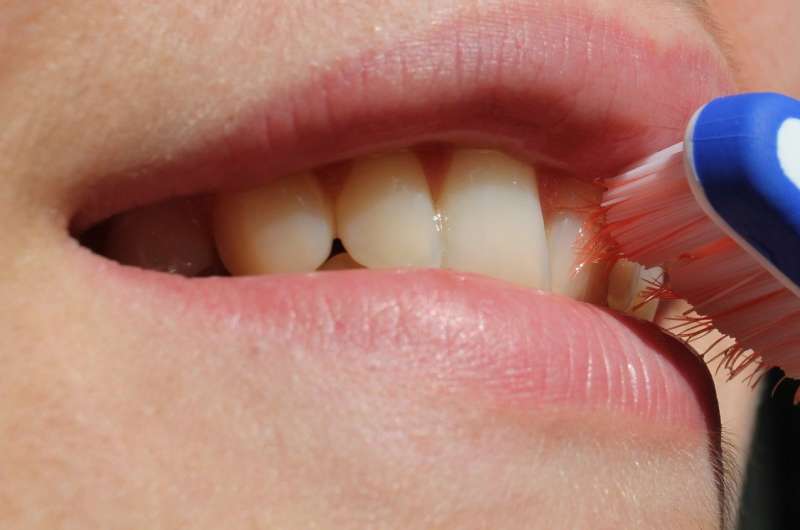
(Medical Xpress)—An international team of researchers has found evidence that suggests certain types of oral bacteria may cause or exacerbate bowel disorders. In their paper published in the journal Science, the group describes testing the impact of introducing bacteria found in the mouths of humans to mice models. Xuetao Cao with the Chinese Academy of Medical Sciences offers a Perspective piece on the work done by the team in the same journal issue and suggests that the work might one day lead to the development of new kinds of treatments for common bowel disorders.
Bowel disorders such as irritable bowel syndrome, ulcerative colitis and Crohn's disease are more than just a nuisance— they can cause serious degradation to quality of life, and in some cases, can even be deadly. For that reason, medical scientists search for answers surrounding their causes and ways to treat them. In this new effort, the researchers report finding a possible link between bacteria that normally live in the mouth and common bowel disorders.
The researchers report that their study began when team members noticed that patients with one of the three main types of bowel disorders also had higher than normal levels of oral bacteria in their feces, suggesting higher levels in their guts. Suspecting there may be a link, the group conducted several experiments to help them learn more about the connection between the two types of bacteria.
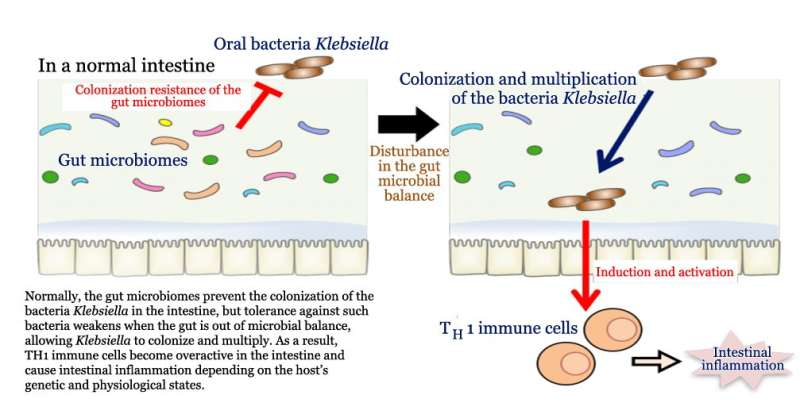
In the first experiment, the researchers introduced human saliva from people with Crohn's disease into the guts of mice with a sterilized gut microbiome. Doing so, they found, led to gut inflammation in some cases. A closer look revealed the bacteria responsible for the inflammation was Klebsiella pneumoniae, a strain commonly found in the human mouth, but seldom in the gut. In another experiment, the researchers introduced the bacteria directly into the intestines of healthy mice and found it caused no problems. Giving the mice Klebsiella-resistant antibiotics once again caused inflammation when Klebsiella was introduced. Other experiments with saliva from colitis patients offered similar results.
As Cao notes, the results suggest there may be a link between the oral bacteria and bowel disorders—more work is required to prove the case, but if it turns out to be true, a future treatment for such disorders may include giving patients oral disinfectants.
More information: Koji Atarashi et al. Ectopic colonization of oral bacteria in the intestine drives TH1 cell induction and inflammation, Science (2017). DOI: 10.1126/science.aan4526
Abstract
Intestinal colonization by bacteria of oral origin has been correlated with several negative health outcomes, including inflammatory bowel disease. However, a causal role of oral bacteria ectopically colonizing the intestine remains unclear. Using gnotobiotic techniques, we show that strains of Klebsiella spp. isolated from the salivary microbiota are strong inducers of T helper 1 (TH1) cells when they colonize in the gut. These Klebsiella strains are resistant to multiple antibiotics, tend to colonize when the intestinal microbiota is dysbiotic, and elicit a severe gut inflammation in the context of a genetically susceptible host. Our findings suggest that the oral cavity may serve as a reservoir for potential intestinal pathobionts that can exacerbate intestinal disease.
© 2017 Medical Xpress











.jpg)