Mass. panel reviews cataract surgery adverse events, makes recommendations for prevention
A team of specialists in anesthesiology, ophthalmology and patient safety convened in response to a series of injuries to patients receiving cataract surgery has reported its findings regarding factors contributing to those and other adverse events and strategies for preventing patient harm in such procedures. In two papers published online in Anesthesia & Analgesia, investigators from the Betsy Lehman Center for Patient Safety, a Massachusetts state agency, detail adverse events associated with cataract surgery in the state over a five-year period, pinpoint factors underlying those events and make recommendations for improvements in patient safety. These papers expand on the expert panel report published by the Betsy Lehman Center in May 2016.
"No medical procedure is immune from human error, and cataract surgery - one of the safest and most commonly performed procedures in the country - offers a clear case in point," says Karen Nanji, MD, MPH, of the Massachusetts General Hospital Department of Anesthesia, Critical Care and Pain Medicine, corresponding author of both papers. "In medicine, it's virtually impossible to eliminate 100 percent of errors, since advances such as new medications and procedures bring new opportunities for errors. So it's critical to continuously evaluate and identify opportunities for improvement."
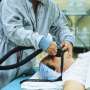
The impetus for the panel's formation was an increase in the number of cataract-surgery-related adverse events reported to the state in 2014. Among those affected were five cataract surgery patients treated on the same day in one facility, several of whom suffered permanent vision loss in the eye that had been operated on. All five patients had received eye blocks - an anesthetic procedure in which medication is injected into the area around the eye to block pain and prevent motion of the eye - from the same anesthesiologist, who was not a regular staff member at the center; and it appeared that the injections had penetrated the patients' eyeballs.
The 12-person panel made up of anesthesiologists, ophthalmologists, medical administrators, patient safety experts and patient representatives reviewed all cataract-surgery-associated adverse events reported to the Mass. Department of Public Health (DPH) or the Quality and Patient Safety Division of the state Board of Registration in Medicine from 2011 through 2015. Of 37 reported events, 15 involved implanting a lens that should have been given to a different patient, 10 were complications from eye blocks, 5 involved eye blocks administered to the wrong eye, 3 involved an inflammatory reaction that is a known complication of the procedure, 2 involved retention of an object or tissue in the surgical area, and 2 involved surgery on either the wrong eye or the wrong patient.
Based on that information, on interviews with additional stakeholders - including cataract surgeons, other specialists and staff members at centers reporting the events - and on a survey of cataract surgeons and facilities, the team determined that the causes of events fell into two categories: system failures and the choice of anesthesia techniques. System failures included inadequate or poorly adhered to safety protocols; communication challenges, including miscommunication among staff and with patients; insufficient training, including inadequate orientation for new or visiting staff and lack of eye-surgery-specific training for anesthesiology residents; and lack of standardization within and between centers for things like storage and labeling of lenses and the marking of surgical sites.
While 15 of the 37 adverse events reported in Mass. were related to eye blocks, the team noted that none of the events involved the use of topical anesthetics or general anesthesia. While a significant number of the surgeons and centers responding to the surveys reported increasing their use of topical anesthesia in the past 10 years, more than 40 percent of procedures were still performed using eye blocks. Fewer than 20 percent of responding surgeons reported "often" or "always" offering patients a choice of anesthesia.
Based on these findings, the team recommended several strategies for reducing the occurrence of adverse events. The most important of these, according to Nanji are:
- use of standardized safety protocols, such as safety checks and clearly marking the surgical site,
- ensuring that all providers are properly trained and oriented to the procedures and resources at each facility,
- use of the least invasive form of anesthesia appropriate to the patient.
"Errors leading to significant patient harm can occur even during procedures as common as cataract surgery, and we must do more to prevent them," says Nanji, an assistant professor of Anesthesia at Harvard Medical School. "It is ultimately the responsibility of health care facilities and care teams to implement prevention strategies. However, if patients scheduled for cataract surgery are concerned, they can ask their surgeon or anesthesiologist about their standard safety protocols - including how they ensure the procedure will be performed on the correct eye - whether they are candidates for less invasive forms of anesthesia, such as the use of eye drops to numb the eye; and how many times a physician has performed a procedure, including an eye block, which we recommend be done under supervision at least 10 times."
More information: Karen C. Nanji et al, Preventing Adverse Events in Cataract Surgery, Anesthesia & Analgesia (2017). DOI: 10.1213/ANE.0000000000002529