Tiny bilirubin-filled capsules could improve survival of transplanted pancreatic cells
By encapsulating bilirubin within tiny nanoparticles, researchers from North Carolina State University and the Ohio State University have improved the survival rates of pancreatic islet cells in vitro in a low-oxygen environment. The work has implications for the treatment of Type 1 diabetes in both canine and human patients.
Patients with Type 1 diabetes are unable to produce enough insulin naturally. One treatment for Type 1 diabetes is pancreatic islet transplantation, in which groups of cells from a donor pancreas are transplanted into the patient—where they can sense glucose levels and produce insulin to control diabetes. Islet transplantation is currently the only non-invasive curative treatment for the disease; however, the main drawback is the high rate of cell death after transplantation.
Unlike an organ transplant, where the organ is connected directly to blood vessels and has an immediate oxygen supply, transplanted islet cells are simply injected into the recipient's bloodstream and lodge in small veins in the liver, a low-oxygen environment in which up to 70 percent of the transplanted cells die within 72 hours of the procedure.
Chris Adin, currently an associate professor of soft tissue and oncologic surgery at NC State's College of Veterinary Medicine and previously at Ohio State, thought that the answer to saving these transplanted islet cells might lie in a naturally occurring antioxidant - bilirubin. "Bilirubin is a molecule found in every cell in our body," says Adin, "and while too much of it can be harmful, it can be beneficial if we supplement cells with just the right amount of this molecule."
So Adin set out to see if adding bilirubin to the islet cells would increase their transplant survival rates. The main obstacle was in delivering the bilirubin to the cells of interest. Since the molecule is not very soluble in water, it couldn't be effectively taken up by the cells if it was simply added to the solution they were in.
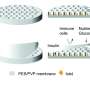
Xiaoming He, professor of biomedical engineering at Ohio State, partnered with Adin to design a delivery vehicle for the bilirubin. They came up with a nanocapsule made from Pluronic 127-chitosan that would enclose the bilirubin molecule, be taken up by the islet cell, and release the bilirubin inside the cell.
He and Adin tested their particles in vitro on islet cells that had been grown in culture and exposed to low-oxygen environments. They found that a dose of 5 micromolar bilirubin had the maximum protective benefit while still preserving the islet cells' function. In those treated cells, the low-oxygen death rate was only 18 percent.
"The cell death rate from islet transplants has been the major roadblock to this procedure's usefulness," says Adin. "These nanocapsules provide a bilirubin delivery method that allows targeted dosing, preserving both the cells and their functionality."
Adin's next steps include creating a treatment program for canine patients which can serve as a model for humans. "There are between 400,000 and 800,000 dogs in the U.S. with Type 1 diabetes," he says. "Figuring out a treatment for dogs will not only alleviate their suffering, but could lead to improved treatments for humans as well."
The work appears in the journal Cell Transplantation.
More information: Bronwyn Fullagar et al, Nano-Encapsulation of Bilirubin in Pluronic F127–Chitosan Improves Uptake in β Cells and Increases Islet Viability and Function after Hypoxic Stress, Cell Transplantation (2017). DOI: 10.1177/0963689717735112