New insights into treating a rare leukemia
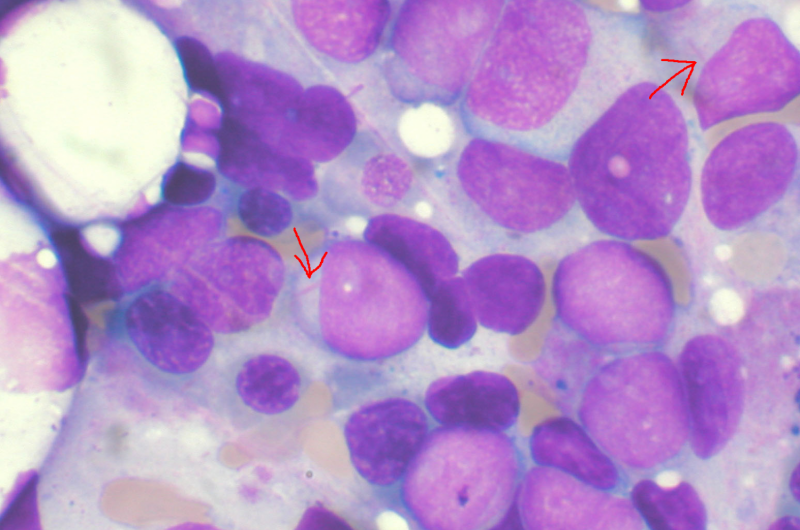
A study at Children's Hospital Los Angeles is shedding new light on the best therapeutic approach for a rare and aggressive leukemia called mixed phenotype acute leukemia (MPAL).
The study—a quantitative synthesis of 20 years of scientific literature—found that starting MPAL treatment with a less-toxic regimen is associated with clear benefits for achieving remission and possibly for long-term survival. The findings were published online in the journal Leukemia on February 27, 2018.
MPAL accounts for 2 to 5 percent of leukemia cases and has been historically difficult to treat, with five-year survival rates of less than 50 percent. The disease affects both children and adults and contains characteristics of two more-common forms of leukemia: acute lymphoblastic leukemia (ALL) and acute myeloid leukemia (AML).
Physicians must decide whether to treat patients with therapy for ALL or therapy for AML, or a hybrid of both approaches. The problem: There's no clear consensus on which approach is best.
"Because this disease is so rare, we haven't had clinical trials with thousands of patients to define the optimal therapy," says Etan Orgel, MD, MS, a specialist in MPAL and a physician in the Center for Cancer and Blood Diseases at Children's Hospital Los Angeles. "Instead, we have many small, isolated and often-conflicting case reports published in widely diffuse journals around the world. It's disjointed."
To make better sense of the available research and provide clearer treatment guidance for physicians, Orgel and a team of CHLA researchers embarked on the first-ever systematic review and meta-analysis of observational studies on MPAL. The team searched more than 17,000 published studies, eventually narrowing that list to 252 relevant papers from 33 countries covering 1,499 patients. Their review included studies using both the European Group and World Health Organization definitions of MPAL.
Their key finding: Patients initially treated with ALL therapy—a significantly less-toxic regimen—were three to five times more likely to achieve a complete remission than AML-treated patients.
Patients starting with ALL chemotherapy were also twice as likely to survive—but that benefit was only found in studies reporting patient results as a group. In studies reporting individual patient results, survival was similar in both the ALL and AML groups—a puzzling discrepancy researchers could not explain. Patients given hybrid therapy, though, fared the worst.
"This makes a really convincing case that starting with ALL therapy is beneficial on all fronts, from remission to overall survival—if not from increasing survival, then from decreasing side effects," says Maria Maruffi, MD, the first author on the study.
Researchers say the next step is a national clinical trial for this rare disease.
"This research provides key insights to help guide physicians treating patients walking in the door today," says Orgel, associate professor of Clinical Pediatrics at the Keck School of Medicine of the University of Southern California. "But it also highlights the critical need for a clinical trial to definitively determine the best therapy for MPAL and help move treatment for this rare disease forward."
More information: Maria Maruffi et al, Therapy for children and adults with mixed phenotype acute leukemia: a systematic review and meta-analysis, Leukemia (2018). DOI: 10.1038/s41375-018-0058-4