February 15, 2018 report
Ketamine found to reduce bursting in brain area reducing depression quickly
A team of researchers at Zhejiang University in China has found that the drug ketamine reduces neuronal bursting in the lateral habenula (LHb) brain region, reducing symptoms of depression in rodent models. In their paper published in the journal Nature, the group describes their study of the impact of the drug on depression and why they believe it may lead to a better understanding of the condition.
Prior research has shown that the drug ketamine, generally used as an anesthetic drug, can lead to reduced symptoms of depression in some people. In this new effort, the researchers have delved farther into the brain to find out why.
The efforts by the team actually resulted in two papers, both printed in Nature. In the first, they report finding that ketamine reduces depression symptoms by blocking LHb neural bursting (where groups of nerves fire as a barrage rather than as a slow pulse). They also noted that for the drug to work, both N-methyl-d-aspartate receptors and low-voltage-sensitive T-type calcium channels had to be active. In their second paper, they describe identifying a possible means for regulating the bursting behavior, reducing the need for blockers such as ketamine.
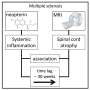
The results explain why ketamine works so quickly, in as little as 30 minutes, to reduce depression symptoms, while other drugs can take weeks or months. Instead of causing changes in brain chemical levels, ketamine simply blocks neural bursting, preventing the brain from making itself depressed. Prior research has shown that LHb is involved in inhibiting reward activation in the brain and is one part of the brain believed to be at least in part responsible for learning from bad experiences. If monkeys taught to pull a lever for a treat are denied a reward, the LHb gets involved, telling the brain not to be so excited about getting a treat. That helps the monkey learn to stop pulling the lever.
The work by the team is preliminary, done with rodents engineered to have depression-like symptoms. Thus, it is not known yet if the same processes are occurring in the human brain. But if the similarities hold up, the team believes their findings could lead to drugs such as ketamine being used to treat depression much more quickly than is available now.
More information: Yan Yang et al. Ketamine blocks bursting in the lateral habenula to rapidly relieve depression, Nature (2018). DOI: 10.1038/nature25509
Abstract
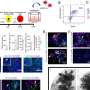
The N-methyl-D-aspartate receptor (NMDAR) antagonist ketamine has attracted enormous interest in mental health research owing to its rapid antidepressant actions, but its mechanism of action has remained elusive. Here we show that blockade of NMDAR-dependent bursting activity in the 'anti-reward center', the lateral habenula (LHb), mediates the rapid antidepressant actions of ketamine in rat and mouse models of depression. LHb neurons show a significant increase in burst activity and theta-band synchronization in depressive-like animals, which is reversed by ketamine. Burst-evoking photostimulation of LHb drives behavioural despair and anhedonia. Pharmacology and modelling experiments reveal that LHb bursting requires both NMDARs and low-voltage-sensitive T-type calcium channels (T-VSCCs). Furthermore, local blockade of NMDAR or T-VSCCs in the LHb is sufficient to induce rapid antidepressant effects. Our results suggest a simple model whereby ketamine quickly elevates mood by blocking NMDAR-dependent bursting activity of LHb neurons to disinhibit downstream monoaminergic reward centres, and provide a framework for developing new rapid-acting antidepressants.
© 2018 Medical Xpress