Scans could help tailor pancreatic cancer treatment
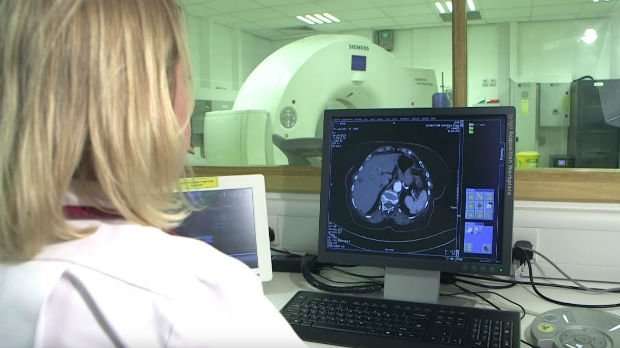
Doctors should use a specialised type of scan to help decide if patients with pancreatic cancer may benefit from surgery, according to the National Institute for Health and Care Excellence (NICE).
New guidance from NICE says a PET-CT scan should be used early in the process of diagnosing pancreatic cancer. It is thought that the scans will give doctors more accurate information on how advanced the disease is.
Professor Mark Baker, director of the centre for guidelines at NICE, said giving patients the PET-CT scan could have a significant impact on the treatment of patients with pancreatic cancer.
"It will mean that the staging process is more effective so that patients stand a better chance of getting the right treatment, at the right time," he said.
Deciding on treatment
Around 9,600 people in the UK are diagnosed with pancreatic cancer each year and survival is stubbornly low.
Surgery is most effective for patients if their disease has been diagnosed early.
NICE estimates that using the PET-CT scan to determine the stage of pancreatic cancer will reduce the number of NHS surgeries to remove these tumours by around 20%. This means that patients with more advanced pancreatic cancer will not undergo surgery that they are unlikely to benefit from.
This would help limit the side effects of surgery. And NICE said those who are not suitable for surgery will then be able to access chemotherapy treatment sooner.
It could also then free up theatre time for other patients.
Professor Andrew Biankin, Cancer Research UK's pancreatic cancer expert, approved of the new guidelines and said they were "an important step forward in making treatment selection for pancreatic cancer patients more precise."
How does a PET-CT work?
A PET-CT scan is a type of imaging machine that combines a CT scan and a PET scan. It gives doctors detailed information about a person's cancer, including the size of the tumour and whether it has spread.
The CT scan takes a series of x-rays around the body and the PET scan uses a radioactive drug to highlight areas in the body where cells are more active than normal.
Biankin added that more research was needed to look at how to better personalise pancreatic cancer treatment.
"We now need to work on better ways to select the best treatment for an individual, which will require testing and imaging at a molecular level," he said.
"At Cancer Research UK, our Flagship Programme PRECISION Panc, based in Glasgow, is working on ways to do just that.
"This programme aims to find the right clinical trial for the patient by offering cutting edge molecular testing of their cancer. The patient can then take part in a trial that's testing out new drugs that better match their individual tumour."
More information: Paula Ghaneh et al. PET-PANC: multicentre prospective diagnostic accuracy and health economic analysis study of the impact of combined modality 18fluorine-2-fluoro-2-deoxy-d-glucose positron emission tomography with computed tomography scanning in the diagnosis and management of pancreatic cancer, Health Technology Assessment (2018). DOI: 10.3310/hta22070