Non-invasive technology is a money-saver for heart patients needing PCI
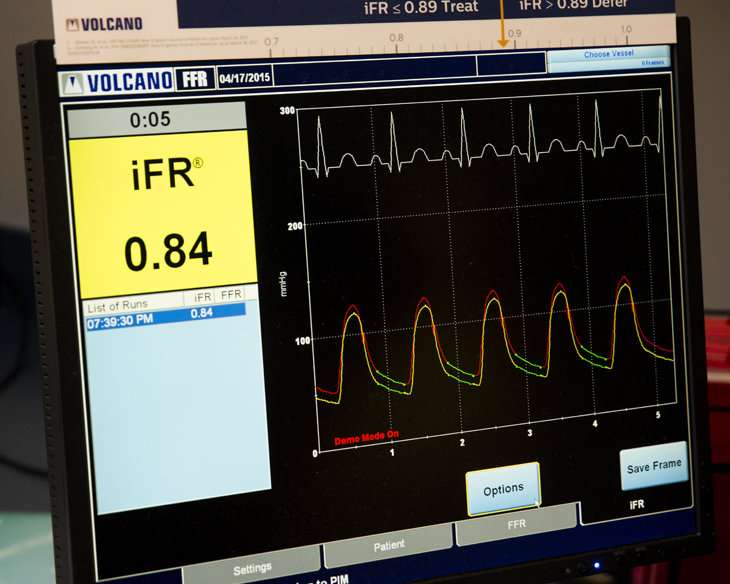
Doctors evaluating patients for blockages in the heart are aided by having a good roadmap of the vascular terrain before they can insert stents to clear the impasse.
Two technologies have been used with equal success, but now a study presented March 10 at the American College of Cardiology annual meeting by Duke cardiologists shows that the newer method carries a much lower cost, potentially saving each patient at least $800.
In a study of nearly 2,500 heart patients, researchers found that a new technology, non-invasive instantaneous wave-free ratio (iFR), was less expensive than an older technology known as fractional flow reserve (FFR), which requires injection of a drug that dilates the blood vessels, adding complexity, expense and potential risk.
"There are clear clinical advantages to using these technologies to map coronary physiology prior to coronary revascularization procedures, because they provide an accurate evaluation of the blockage, as well how best to treat it," said senior researcher Manesh Patel, M.D., chief of the Division of Cardiology at Duke and member of the Duke Clinical Research Institute. "Unfortunately, there has been resistance to performing FFR in part due to the use of the vasodilator drug, so finding a good alternative is an important clinical step."
Patel said iFR has in recent years emerged as an alternative in recent years. Unlike FFR—which requires administration of the drug adenosine to maximally vasodilate the heart muscle and then measure the differences in a pressure along a blocked or narrowed artery—iFR relies on measuring the pressure during a specific point in the cardiac cycle.
A study called DEFINE-FLAIR compared iFR to FFR and reported last year that the different technologies performed similarly for clinical outcomes, with iFR actually resulting in fewer symptoms for patients before, during and after the procedure.
In the current study, the question was whether iFR might be less expensive than FFR, which would eliminate another potential barrier to its use. Using the DEFINE-FLAIR data for their cost analysis, Patel and colleagues found that the average cost of the catheterization procedure was lower in the iFR group than in the FFR group, at $2,489 vs. $2,564.
The iFR procedure was less costly because it took less time, didn't require the vasodilation drug, and resulted in lower percutaneous coronary intervention rates.
Patients in the iFR group also had significantly fewer coronary artery bypass graft procedures and fewer subsequent revascularisations than those in the FFR group.
Overall, health care costs were estimated at $7,442 with iFR and $8,243 with FFR, for an unadjusted saving of $801 per patient.
"Either of these two technologies improve outcomes for patients with coronary disease, but our study shows that iFR has cost savings with similar outcomes," Patel said. "This should help remove barriers to the more widespread clinical adoption of a technology that can provide physicians with a better conception of patients' unique coronary physiology."