Human insulin as safe and effective to treat type 2 diabetes as costlier insulin analogs
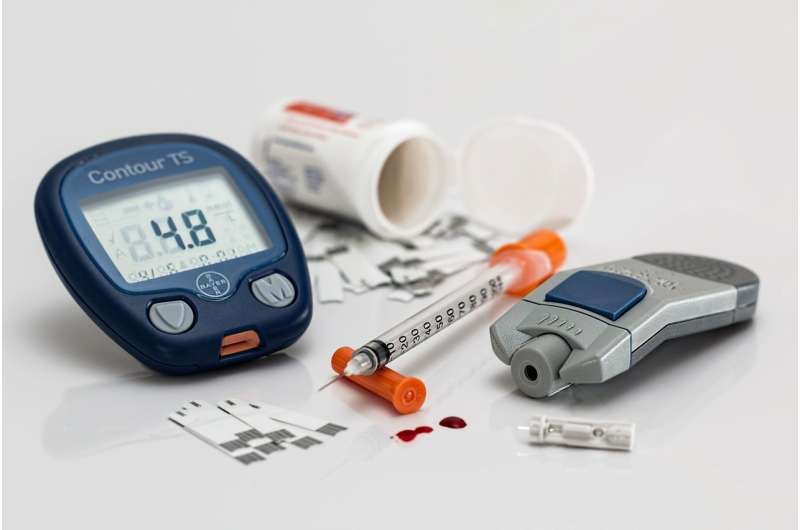
Patients with Type 2 diabetes who were treated with the newer generation of insulin analog drugs did not have substantially better outcomes than those treated with less costly human insulin, according to a study by Yale School of Medicine researchers and colleagues at Kaiser Permanente.
The study is published in the June 23 issue of Journal of the American Medical Association.
"We compared the newer and older types of insulin in a large and diverse population of Kaiser Permanente type 2 diabetes patients who were newly prescribed insulin," said lead author Kasia J. Lipska, M.D., assistant professor of medicine at Yale School of Medicine. "The study was conducted under real-world conditions with uniquely detailed data about possible confounding factors and long-term outcomes."
"We found that for patients with type 2 diabetes in usual practice, the use of the more expensive insulin analogs did not appear to result in better safety—at least as defined by hospital or emergency visits for hypoglycemia—or better blood sugar control compared with NPH insulin," Lipska added. "This suggests that many people with type 2 diabetes should consider starting with NPH insulin, instead of insulin analogs, especially if cost is an issue for them."
For the estimated 29 million Americans with diabetes, treatment of type 2 diabetes typically begins with lifestyle modifications and metformin, a pill that lowers the amount of sugar in the blood. However, up to 25% of diabetes patients eventually require additional insulin injections to control their blood sugar.
"For decades, people initiating insulin treatment were prescribed human insulin," said Andrew J. Karter, senior research scientist with the Kaiser Permanente Division of Research. "Then in the 2000s, a new generation of long-acting insulin analogs emerged that were designed to mimic human insulin."
Like human insulin, long-acting insulin analogs can be prescribed as daily or twice-daily injections to help provide predictable levels of blood sugar throughout the day. In clinical trials, insulin analogs modestly reduced the risk of nocturnal hypoglycemia, or low blood sugar during sleep, compared with human insulin.
"The problem is that insulin analogs are much more expensive than human NPH insulin," said Lipska. A vial of insulin analog now costs about $200 to $300, while a vial of NPH insulin costs just $25. The cost of analog insulin has tripled nationally between 2002 and 2013. Dr. Karter's research has shown that high out-of-pocket cost of medications, especially at the time of initiation, are linked to poorer adherence, which directly affects outcomes for diabetes patients."
To compare insulin analogs with NPH insulin, Lipska, Karter and their colleagues followed the new insulin users with type 2 diabetes for an average of 1.7 years. During this time, they examined emergency department visits or hospitalizations related to severe hypoglycemia, as well as changes in their blood sugar (hemoglobin A1c) control. They found that insulin analogs were not associated with a reduced risk of emergency department visits or hospital admissions for severe hypoglycemia, nor did they control hemoglobin A1c levels better than NPH insulin.
"The cost differential between analog and NPH insulins is huge, up to a 10-fold difference," Karter said. "Some people with type 2 diabetes may find the potential benefits of insulin analogs worth the additional cost. But we found no population-level evidence to suggest that the extra expenditure is warranted for most people with type 2 diabetes, particularly when the high cost could prevent some of them from getting the treatment they need or divert resources away from other, potentially beneficial clinical interventions."
More information: Kasia J. Lipska et al, Association of Initiation of Basal Insulin Analogs vs Neutral Protamine Hagedorn Insulin With Hypoglycemia-Related Emergency Department Visits or Hospital Admissions and With Glycemic Control in Patients With Type 2 Diabetes, JAMA (2018). DOI: 10.1001/jama.2018.7993