Clinics manage hypertension patients better when more hands are on deck
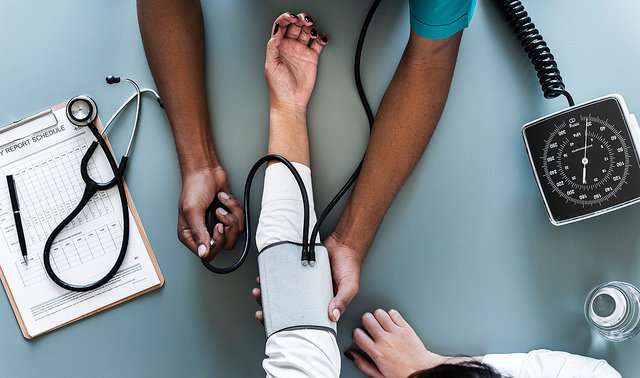
South Africa's clinic based health system was originally created to provide primary care services like maternal and child care and care for acute conditions such as pneumonia or malaria. But the clinics have been facing rapidly increasing demand for a range of additional services. This is partly because of the need to provide antiretroviral drugs at clinic level and partly because there is an increasing number of older South Africans who have chronic conditions like high blood pressure (hypertension).
In 2011, policy makers made changes to the system in clinics to improve the service for chronic conditions like hypertension. This included, for example, getting nurses to pre-pack repeat prescriptions and allowing chronic patients to queue separately from other patients. The aim was to improve the operational efficiency of the clinics to improve quality of care by, for example, shortening queues. But the new system meant that nurses had many more extra administrative tasks and they were struggling to cope.
In our study we explored whether trained, low cost and locally based lay health workers could ease the nurses' administrative load and improve clinic services for hypertension. Our trial -– the first of its kind –- looked at whether the lay health workers would increase the number of people with hypertension accessing care, and ultimately reducing the number of people with uncontrolled hypertension in the community.
Research shows that hypertension affects a great number of adults but that they are often unaware of the condition. As a result, hypertension is poorly controlled. In South Africa, for instance, about 78% of people over the age of 60 suffer from hypertension but only 24% are on treatment.
In the trial the lay health workers took over administrative and educational aspects of care, allowing nurses to focus on the clinical consultations. Our study showed that adding lay health workers to the clinics improved the care that patients received. More patients attended on their appointed day, and their waiting time was reduced by one hour.
But the presence of the lay health workers didn't reduce the number of people in the community who had uncontrolled high blood pressure. We believe that this was due to two connected factors: that nurses were still overwhelmed by the sheer numbers of patients coming to the clinics for treatment, and that faulty equipment like blood pressure machines, meant proper diagnosis couldn't be done.
Our research
Our aim was to test how well the intervention could work in a routinely functioning health care system.
We conducted our trial between 2014 and 2015 at eight clinics in Mpumalanga – one of South Africa's mainly rural provinces in the north east of the country. Lay health workers were employed at four clinics and the other four continued with their usual care. The main aim was to measure differences in the functioning of these two sets of clinics and how hypertension was controlled in the communities.
Lay health workers were recruited from local villages and paid similar salaries to community health workers. They were supervised by a local professional nurse and worked in the clinics alongside staff who decided how the lay health workers could help. They booked appointments, reminded patients of their appointments, filed patient records, provided education on healthy lifestyles and the importance of adhering to treatment, measured vital signs and assisted nurses to pre-pack medication.
To evaluate their impact two population-wide surveys were done. The first took place before the lay health workers joined the clinics and the other 18 months later after they finished their work.
In addition to the population surveys, we interviewed patients, community members, nurses and managers. We also evaluated the clinics to understand how the intervention was working. And we collected clinical data about patients with chronic diseases who attended the clinics during the trial.
Our findings
We made two significant findings: there was no difference between the two sets of clinics when it came to the proportion of the population with uncontrolled hypertension and cardiovascular risk. But there were significant improvements in the functioning of clinics that had recruited lay health workers. Their presence improved the way that hypertension was managed in several ways. This included:
- increases in the number of patients being treated for hypertension.
- more patients attending the clinic on the correct appointment day because lay health workers reminded them about their appointments.
- reducing the waiting time for patients by around one hour because they retrieved patients' files before they came and assisted nurses by pre-packing medication and measuring vital signs, and
- nurses being relieved of some routine work like booking patients of their appointments.
Despite the help from the lay health workers, there were still several challenges at the clinics.
They struggled with the rapidly increasing number of chronic disease patients; the patient load increased by about 75% over the 18 month period.
And there were infrastructure problems such as cramped buildings and unreliable blood pressure machines.
There were also logistical challenges. The supply of drugs was erratic and keeping good clinic records was difficult because there were often no files to write in and photocopiers were mostly not working.
Hypertension treatment took lower priority than HIV treatment because the anti-retroviral programme was funded, monitored and managed separately from other clinic activities, with the result that the HIV treatment programme received more attention.
Part of a functioning system
Our study shows that adding additional human resources – even if they are readily available and relatively inexpensive – is unlikely to have a positive effect on health if the necessary equipment to accurately measure blood pressure is not available and if there aren't enough clinical staff to treat the growing numbers of chronic patients.
This article was originally published on The Conversation. Read the original article.![]()