Saliva test could improve diabetes control and treatment
Diabetes assessment currently relies on measurement of blood sugar levels—but a simple saliva sample could replace this, says new research. The study, published in Frontiers in Physiology and the most comprehensive of its kind to date, finds that proteins in saliva reflect high blood sugar and associated disease processes in young patients with type 1 diabetes, long before the appearance of clinical symptoms. This could lead to better prediction and prevention of long-term complications of the disease.
People with type 1 diabetes produce too little insulin. This hormone is required for the body to use sugar for energy, so lack of insulin causes unused sugar to accumulate in the blood. This excess sugar in turn leads to complications like cardiovascular, kidney, eye and nerve damage.
With no known cure for type 1 diabetes, the key to preventing these complications is careful control of blood sugar levels. This is achieved with insulin injections—balanced with lifestyle factors like diet and exercise—and requires regular blood testing to monitor sugar control.
But this invasive monitoring can be problematic, particularly in children and adolescents.
"Blood collection through repeated sampling causes discomfort and hinders patients' compliance," explains study co-author Professor Heleni Vastardis of NKU Athens School of Dentistry. "Easy, simple, painless, non-invasive saliva collection is the most attractive diagnostic medium when examining children."
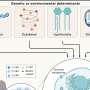
Our saliva contains thousands of proteins produced by our salivary glands and gums, with important roles like healing, digestion and fighting disease. Previous research shows that the amounts of each of these proteins—collectively called the "salivary proteome"—differ between healthy people and those with diabetes.
Vastardis and colleagues see great potential in this finding. "Saliva is considered a mirror of the body's health and disease and a possible game changer in healthcare and clinical practice," she says.
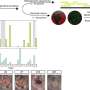
Their new study is the most comprehensive characterization of the salivary proteome to date. It analysed saliva samples from young type 1 diabetics with satisfactory or poor blood sugar control and from matched healthy subjects, using a highly sensitive technique to identify and quantify more than 2,000 different proteins.
The researchers found that young type 1 diabetics with good blood sugar control had similar saliva protein profiles to non-diabetics.
In contrast, young people with poorly controlled type 1 diabetes showed a very different saliva protein profile. The differences were in proteins known to have key roles in inflammation, clotting and blood vessel function—processes that are disrupted by high blood sugar and thereby underly the major long-term complications of diabetes.
Crucially, none of these young patients yet had any clinical signs of eye, kidney or nerve damage. "In other words, the signs of diabetic pathology are already in place way before manifestation of clinical complications," Vastardis points out.
This suggests that the diabetic salivary proteome could be used to predict complications—and help prevent them. "Salivary diagnostics enable the assessment of asymptomatic diabetic patients and the identification of high-risk patients likely to face diabetic complications. This knowledge may offer access to novel points of intervention."
To demonstrate this principle, the group used their results to identify a potential new preventive treatment for young patients with poor diabetic control. By searching a gene database, they found a drug candidate capable of reversing the salivary proteome changes associated with high blood sugar.
This proof-of-concept study demonstrates the power of salivary protein analysis in diabetes research—and soon in the diabetes clinic, Vastardis believes.
"We envision that in the near future we will be able to diagnose and monitor therapeutic strategies in diabetes with only a drop of saliva, through ultra-sensitive and highly specific techniques such as the Multiple Reaction Monitoring used in our study as well as real-time, non-invasive, salivary glucose monitoring devices."
"However, larger cohorts are required to completely utilize the information and to account for the potential variance."
More information: Eftychia Pappa et al, Saliva Proteomics Analysis Offers Insights on Type 1 Diabetes Pathology in a Pediatric Population, Frontiers in Physiology (2018). DOI: 10.3389/fphys.2018.00444