At-risk teens and young adults overlooked during opioid crisis
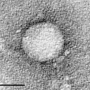
Teens and young adults who have injected drugs are at risk for contracting hepatitis C, but most aren't tested and therefore don't receive life-saving treatment, according to a national study being presented at IDWeek 2018. The study of more than 250,000 at-risk youth found only one-third of those with diagnosed opioid use disorder (OUD) were tested for hepatitis C.
This study is the first to look at opioid use and hepatitis C testing in at-risk youth. "We're missing an opportunity to identify and treat young people who are at risk for this deadly infection," said Rachel L. Epstein, MD, MA, lead author of the study and a post-graduate research fellow in the section of infectious diseases, Boston Medical Center. "Screening for OUD and other drug use, and then testing for hepatitis C in those at high risk, can help us do a better job of eliminating this serious infection, especially now that very effective hepatitis C medications are approved for teenagers."
An infection of the liver, hepatitis C killed more than 18,000 Americans in 2016, making it the most common cause of death from a reportable infectious disease, according to the Centers for Disease Control and Prevention (CDC). It can be spread by sharing needles used to inject drugs. Health care providers may not test young people they suspect of misusing opioids because the drugs are available in pill form, which does not increase the risk of infection with hepatitis C. But studies show many youths who misuse prescription oral opioids eventually begin injecting them. Results of the study suggest that current guidelines—which only recommend testing those with known injected drug use or other specific risk factors—underestimate who is at risk for hepatitis C.
In 2017, the Food and Drug Administration (FDA) approved the first direct-acting hepatitis C medications for teens. These medications can cure a person with hepatitis C infection in two to three months. Without treatment, people may develop liver failure, liver cancer, or chronic liver disease (cirrhosis) many years after being infected.
For the study, researchers analyzed electronic medical records for 269,124 teens and young adults (13-21 years old) who visited one of 57 Federally Qualified Health Centers, which provide health care to diverse and underserved communities across 19 states, between 2012 and 2017. Of the 875 who had diagnosed OUD, 36 percent were tested for hepatitis C, and of those, 11 percent had been exposed to hepatitis C and 6.8 percent had evidence of chronic hepatitis C infection.
Overall, 6,812 (2.5 percent) who visited the health centers were tested for hepatitis C and of those, 122 (1.8 percent) tested positive for hepatitis C. Researchers found those most likely to be tested for hepatitis C were African American youth, those with any substance use disorder, and those 19-21 years old.
"The issue is complicated by the fact that not enough at-risk youth are screened for opioid or other drug use for a variety of reasons, including lack of time, comfort level between clinician and patient, and privacy and stigma concerns," said Dr. Epstein. "And even when drug use is identified, there's a belief that youth are less likely to test positive for hepatitis C, which isn't necessarily the case as we show in our study. Clearly, this is an overlooked group that is at high risk."