Supply chain transparency needed to combat soaring insulin costs
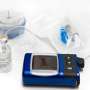
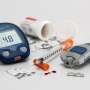
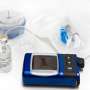
Spiraling insulin costs have created a dangerous barrier for many people with diabetes who need to access lifesaving treatments. The Endocrine Society is calling on stakeholders across the supply chain to help reduce out-of-pocket costs for people with diabetes.
More information about the factors driving cost increases is needed to effectively combat the trend, the Endocrine Society said in a position statement issued today. The complex interactions among insulin manufacturers, pharmacies, health plans, pharmacy benefit managers (PBMs), and wholesalers make it challenging to determine where in the supply chain costs continue to soar. The cost of insulin has nearly tripled in the past 15 years.
The current climate makes it difficult, if not impossible, to understand how much each stakeholder gains when costs to the patient increase. Research indicates that the net price increase insulin manufacturers earn has risen at a far slower rate than insulin list prices.
"Without clear information about expenses incurred by various players in the supply chain, we cannot fully understand what is driving costs up or how to best reduce insulin costs for people with diabetes in the future," said Society spokesperson Rita R. Kalyani, M.D., Associate Professor of Medicine at Johns Hopkins University School of Medicine. "High costs are forcing some people with diabetes to make the life-threatening decision to ration insulin. This is unacceptable for optimal patient care. Everyone needs to be part of the solution to this problem."
In its statement, the Society recommended policy changes to help increase access to affordable insulin, including:
- Future list price increases should be limited, and reasonable financial incentives should be pursued by all stakeholders.
- Patients' share of costs should be limited to a co-pay, and human insulins should be available at no cost to the patient.
- Rebates should be passed along to consumers without increasing premiums or deductibles.
- Healthcare providers should be trained to use lower-cost human insulins and prescribe them as appropriate.
- Patient Assistance Programs should be less restrictive and have an accessible, common application that can be used for multiple programs.
- Electronic medical records should include up-to-date formulary and price information.
- Physicians should consider prescribing the lowest cost insulin when clinically equivalent options are available.
The three insulin manufacturers are taking steps to address this issue. Insulin manufacturer Sanofi announced today it is expanding its VALyou Savings Program to include nearly all of its insulins. The program offers the company's insulins at one set price: $99 for a 10 mL vial or $149 for a box of pens. The company's combination insulin product is not included in the program. This summer, Eli Lilly launched a patient-focused helpline to help individuals with high out-of-pocket costs reduce their financial burden. Novo Nordisk pledged to limit price hikes in 2016 and has kept annual list price increases in the single digits for the past two years.
The Congressional Diabetes Caucus is evaluating legislative action to address rising insulin costs, and its members held a hearing to examine what is driving cost increases and potential solutions to the problem. The Caucus released findings from its insulin probe today. Congress passed legislation last month that eliminated rules blocking pharmacists from informing patients whether they could purchase their medications for less money. The Trump administration has proposed having Medicare pay for certain medications based on the prices in other industrial nations.
More than 30 million Americans have diabetes, and an additional 84 million have prediabetes. Currently, 7.4 million children and adults use insulin to treat their diabetes. These patients use at least one vial of insulin per month, and some need to purchase multiple vials or multiple types of insulin each month. For people with type 1 diabetes, insulin is the only treatment for their life-long disease. Many people with type 2 diabetes will eventually need insulin treatment as their disease progresses.
Individuals with diabetes need to stick to their medication regimen to avoid unnecessary hospitalizations and complications, but rising insulin costs discourage medication adherence. One study indicates that improved adherence among people with diabetes could prevent nearly 700,000 emergency department visits, 341,000 hospitalizations and save $4.7 billion annually.
As more insurance plans shift to a high-deductible structure, the cost of insulin falls more heavily on consumers. Patient Assistance Programs help some individuals, but they can be difficult to navigate and have been shown to increase medication prices overall. Rebate programs, another effort to reduce costs, are often used by employers to reduce health insurance premiums rather than patients' out-of-pocket costs.