AASM publishes clinical practice guideline on use of PAP therapy for sleep apnea

A new clinical practice guideline from the American Academy of Sleep Medicine (AASM) provides guidance to clinicians on the use of positive airway pressure (PAP) therapy to treat obstructive sleep apnea (OSA) in adults.
The guideline, published in the Feb. 15 issue of the Journal of Clinical Sleep Medicine, provides nine recommendations for PAP treatment of OSA in adults and is intended for use in conjunction with other AASM guidelines in the evaluation and treatment of sleep-disordered breathing. It includes four strong recommendations, which clinicians should follow under most circumstances:
- We recommend that clinicians use PAP, compared to no therapy, to treat OSA in adults with excessive sleepiness.
- We recommend that PAP therapy be initiated using either auto-adjusting PAP (APAP) at home or in-laboratory PAP titration in adults with OSA and no significant comorbidities.
- We recommend that clinicians use either continuous PAP (CPAP) or APAP for ongoing treatment of OSA in adults.
- We recommend that educational interventions be given with initiation of PAP therapy in adults with OSA.
"We, as the task force, believe that readers will find the guideline of value in further supporting the need to use PAP therapy for treatment of adults with obstructive sleep apnea who are excessively sleepy, have concomitant hypertension, or have impaired sleep-related quality of life," said lead author Susheel P. Patil, MD, Ph.D., an assistant professor of medicine and clinical director of the Johns Hopkins Sleep Medicine Program in Baltimore. "Furthermore, we hope the guideline provides the rationale for providers, health systems, and payors to establish programs that promote early and sustained adherence to PAP therapy for the benefit of patients experiencing the consequences of obstructive sleep apnea."
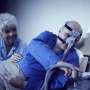
Nearly 30 million adults in the U.S. have obstructive sleep apnea, a chronic disease that involves the repeated collapse of the upper airway during sleep. Common warning signs include snoring and excessive daytime sleepiness. PAP therapy uses mild levels of air pressure, provided through a mask, to keep the throat open during sleep.
Developed by an expert task force and approved by the AASM board of directors, the guideline updated and consolidated previously published practice parameters and was based on a systematic literature review, meta-analyses, and assessment of the evidence using the GRADE methodology. A draft of the guideline was previously made available for public comment.
The guideline includes two good practice statements that the task force considered to be necessary for appropriate and effective patient care: Treatment of OSA with PAP therapy should be based on a diagnosis of OSA established using objective sleep apnea testing, and adequate follow-up should occur following PAP therapy initiation and during treatment of OSA. The guideline also provides five conditional recommendations, which reflect a lower degree of certainty regarding the outcome and appropriateness of the patient-care strategy for all patients.
- We suggest that clinicians use PAP, compared to no therapy, to treat OSA in adults with impaired sleep-related quality of life.
- We suggest that clinicians use PAP, compared to no therapy, to treat OSA in adults with comorbid hypertension.
- We suggest that clinicians use CPAP or APAP over bilevel PAP (BPAP) in the routine treatment of OSA in adults.
- We suggest that behavioral and/or troubleshooting interventions be given during the initial period of PAP therapy in adults with OSA.
- We suggest that clinicians use telemonitoring-guided interventions during the initial period of PAP therapy in adults with OSA.
"Untreated obstructive sleep apnea can have a detrimental impact on a patient's health, well-being and quality of life," said AASM President Dr. Douglas Kirsch. "When obstructive sleep apnea is effectively treated with PAP therapy, many patients report that the impact is life-changing."
The task force found that additional research is needed to evaluate the impact of PAP therapy on cardiovascular risk, neurocognition and mortality. Patil added that a section with additional considerations for clinicians summarizes the evidence with respect to mask selection, humidified PAP, and modified pressure profile PAP, factors that he says may have important implications for clinical practice.
More information: Susheel P. Patil et al, Treatment of Adult Obstructive Sleep Apnea with Positive Airway Pressure: An American Academy of Sleep Medicine Clinical Practice Guideline, Journal of Clinical Sleep Medicine (2019). DOI: 10.5664/jcsm.7640