Vitamin B3 analogue boosts production of blood cells
Stem cell-based therapies are becoming increasingly common, especially in the treatment of blood cancers like lymphoma and leukemia. In these cases, the patient's cancerous blood stem cells are removed and replaced with new, healthy ones. However, up to a quarter of cases end in death because replenishing of blood cells is too slow.
One solution to this is to boost the divisions of so-called hematopoietic ("blood-making") stem cells (HSCs); these are the stem cells that produce the various types of blood cells. Thus, pushing HSCs to divide faster would be ideal; the question is how.
Scientists already know that stress causes HSCs to slow down—reconstituting the entire blood-cell supply system can be overwhelming. In terms of biology, this stress causes increased activity in mitochondria, the energy-producing organelles of the cell.
To meet the high demands of rebuilding blood cells, the mitochondria of the HSCs increase a process called "oxidative phosphorylation," which generates fuel for the cell. But this comes at a cost: Boosting the activity of mitochondria causes HSCs to age prematurely.
A team of scientists led by Olaia Naveiras at EPFL and Nicola Vannini at the Ludwig Institute for Cancer Research Lausanne Branch now report that an analogue of vitamin B3, nicotinamide riboside, can increase HSCs and boost their activity. The study, which also involved labs from EPFL's Institute of Bioengineering, and the University hospital of Lausanne (CHUV), has significant implications for stem-cell therapy patients, especially since nicotinamide riboside can be taken as a dietary supplement and still confer such effects.
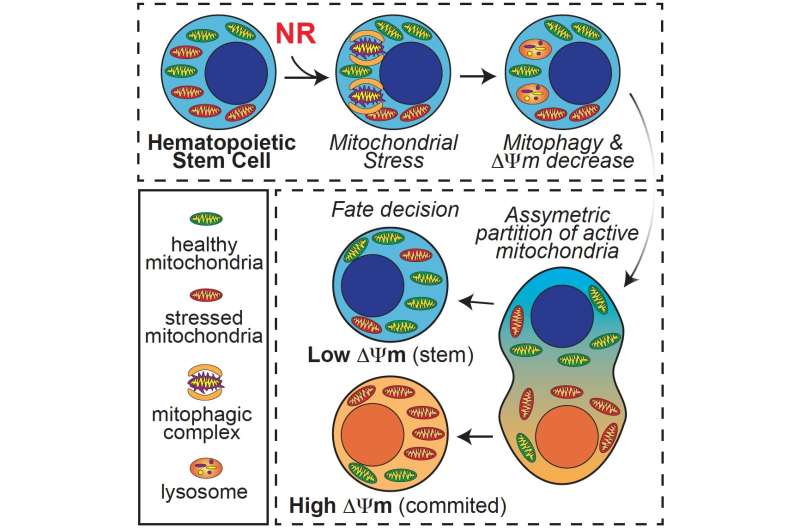
The researchers found that exposing human and mouse HSCs to in vitro nicotinamide riboside improves their function and increases mitochondrial recycling, the process by which stressed-out mitochondria are cleared out to make way for fresh ones. They report that adding nicotinamide riboside to the diet of mice that had undergone an irradiation procedure that eliminates blood cells—modeling radiotherapy—improved their survival by 80 percent and accelerated blood recovery. In immunodeficient mice, nicotinamide riboside increased the production of white blood cells (leucocytes).
This represents a significant improvement in the ability of HSCs to divide and produce new blood cells. The study shows, for the first time, that nicotinamide riboside as a dietary supplement can have a significant positive effect on preventing blood-recovery problems in cancer patients, even after chemo or radiotherapy.
"We expect nicotinamide riboside and other mitochondrial modulators to become a complementary approach for increasing stem cell fitness and accelerating blood production, either through dietary supplementation or pharmacological administration," says Naveiras.
More information: The NAD-booster nicotinamide riboside potently stimulates hematopoiesis through increased mitochondrial clearance. Cell Stem Cell 07 March 2019. DOI: 10.1016/j.stem.2019.02.012