Exploiting metabolic differences to optimize SSRI dosing in adolescents

In a simulated study, exposure to and maximum blood concentrations of two selective serotonin reuptake inhibitors (SSRIs) - commonly used to treat anxiety and depression in adolescents—differed depending on whether the teens modeled were poor, normal, rapid, or ultra-rapid metabolizers of the SSRIs. Caused by differences in the gene coding for cytochrome P4502C19 (CYP2C19), this information could inform SSRI dosing to optimize efficacy of the medications and minimize adverse effects, as reported in an article published in the Journal of Child and Adolescent Psychopharmacology.
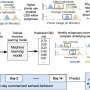
Jeffrey Strawn, MD, University of Cincinnati College of Medicine (OH), Ethan Poweleit, Children's Hospital Medical Center, Cincinnati, and Laura Ramsey, Ph.D., Children's Hospital Medical Center and UC College of Medicine, used pharmacokinetic modeling to compare SSRI exposure and compare the effects of different doses and dosing strategies, such as twice-a-day dosing in individuals who carry forms of the CYP2C19 gene that cause SSRIs to be broken down and cleared from the blood at different rates. In fact, the simulation study showed that in some cases a poor metabolizer might need to be given twice as much drug as a normal metabolizer. The extent of the differences seen within the model were not the same for the two SSRIs compared, escitalopram and sertraline. The researchers describe the study design and present their results in the article entitled "CYP2C19-Guided Escitalopram and Sertraline Dosing in Pediatric Patients: A Pharmacokinetic Modeling Study."
"Anxiety and depression are the most common mental health disorders of adolescence. This study provides important insights for psychiatrists treating adolescents who are non-responsive to SSRI treatment," says Harold S. Koplewicz, MD, Editor-in-Chief of the Journal of Child and Adolescent Psychopharmacology and President of the Child Mind Institute in New York.
More information: Jeffrey R. Strawn et al, CYP2C19-Guided Escitalopram and Sertraline Dosing in Pediatric Patients: A Pharmacokinetic Modeling Study, Journal of Child and Adolescent Psychopharmacology (2019). DOI: 10.1089/cap.2018.0160