Once-per-month HIV drugs on the horizon
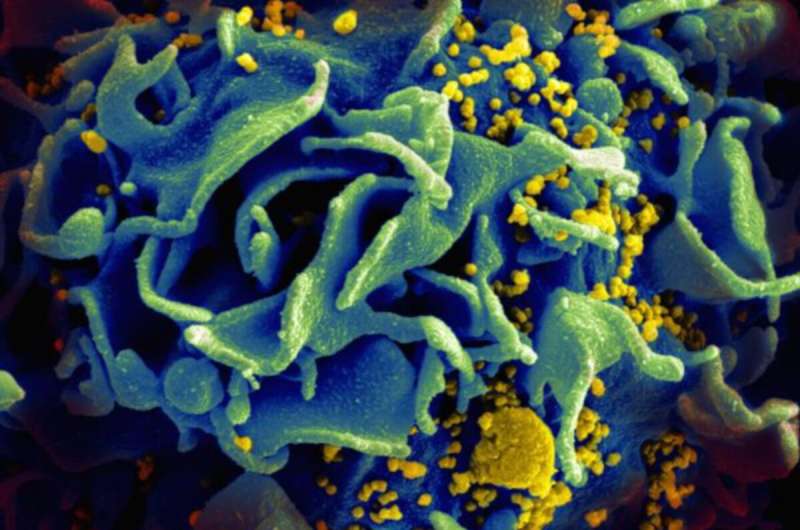
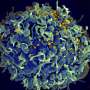
An HIV diagnosis was once a death sentence, but now people who receive treatment survive for decades with the disease. Keeping the virus at bay usually requires taking a pill every day, which aside from being inconvenient for some, is an unwelcome daily reminder of the disease. That's why drug companies are developing longer-acting, injectable HIV treatments, according to an article in Chemical & Engineering News (C&EN), the weekly newsmagazine of the American Chemical Society.
According to the U.S. Centers for Disease Control and Prevention, 38,000 people in the U.S. were newly infected with HIV in 2017. For more than 15 years, the first line of therapy has been a suite of antiretroviral drugs in pill form, taken once a day. Although this treatment has transformed HIV from a certain killer to a chronic disease in much of the developed world, there are problems. For example, some people have trouble taking their pill every day. Therefore, pharmaceutical companies are developing injectable HIV drugs that target different components of the virus and can be administered once every few weeks, writes Senior Editor Megha Satyanarayana.
Currently, at least nine long-acting injectable therapies for HIV are in clinical development. Recently, ViiV Healthcare released data from two Phase III clinical trials of a combination treatment of two drugs that inhibit different parts of the virus. When given as an intramuscular injection, the therapy was as effective as pills and persisted in the body for at least a month. In addition, more than 97% of study participants said in a survey that they preferred the long-acting injectable to daily pills. Other researchers are looking beyond treatment to a possible cure for HIV, developing therapies, such as broadly neutralizing antibodies, that could "wake up" and then kill dormant viruses. Although injectable HIV drugs could be a welcome convenience for many, some experts are skeptical that they would actually improve treatment compliance, especially among people who are homeless or lack stable insurance coverage.
More information: "With several long-acting HIV treatments in the works, the newest drugs emphasize convenience," cen.acs.org/pharmaceuticals/dr … atments-works/97/i19