Radio-frequency heating of hip arthroplasty implants during metal artifact reduction
Clinical metal artifact reduction sequence (MARS) magnetic resonance imaging (MRI) protocols at 3 Tesla (3T) on hip arthroplasty implants pose minimal risk of thermal injury, according to a study to be presented at the ARRS 2019 Annual Meeting, set for May 5-10 in Honolulu, HI.
The study was conducted to investigate the heating effect of clinical and nonclinical MARS MRI protocols at 3T on different hip arthroplasty implants.
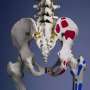
Two American Society for Testing and Materials (ASTM) MRI phantoms—objects developed to stand-in for human tissue during MRI testing and calibration—were used to simulate the upper and lower portions of a human torso. Four total hip arthroplasty implant configurations were tested, including a metal-on-polyethylene construct with cobalt chromium (CoCr) femoral stem, a metal-on-metal construct with CoCr femoral stem, and two metal-on-ceramic constructs with titanium femoral stems at two lengths. Temperature changes of three clinical pulse sequence type protocols were measured, including high-bandwidth turbo spin echo (HBW-TSE), slice encoding for metal artifact correction (SEMAC), and compressed sensing SEMAC (CS-SEMAC). In addition, a 30-minute HBW sequence was modified twice to produce high, "supraclinical," SAR values to assess potential extreme scenarios.
The maximum heating at any single point was 1.9 °C across all three clinical MARS MRI protocols and implant configurations. With supraclinical high SAR pulse sequences at up to 30 min of continuous MRI, heating increased to 3.6 °C.
The results suggest only a minimal risk of thermal injury with the clinical MARS MRI protocols used, especially when adding the cooling effect of perfusion in physiologic conditions.
More information: www.arrs.org/am19