Changes in blood flow tell heart cells to regenerate

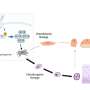
Altered blood flow resulting from heart injury switches on a communication cascade that reprograms heart cells and leads to heart regeneration in zebrafish, says a new study in eLife.
The findings reveal signalling pathways important for heart regeneration in zebrafish that are also present in mammals, providing insights that could help scientists find new ways to repair the organ after a heart attack in future.
Heart muscle cells called cardiomyocytes hold on to the capacity to reprogram themselves and alter their fate in response to heart damage. Although several signalling cues are known to be involved in this regeneration activity, it is not well understood how heart injury switches on these pathways to initiate heart cell reprogramming.
"Recent studies suggest that biomechanical forces generated by blood flow can contribute to heart development through modulating cell signalling," explains lead author Manuel Gálvez-Santisteban, a postdoctoral scientist at the University of California, San Diego (UC San Diego), US. "We wanted to explore this further by seeing whether mechanical forces caused by altered blood flow during heart injury also activate these signalling pathways to control heart cell reprogramming and regeneration."
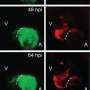
The team first looked at how heart injury affects signalling of an important heart development molecule called Notch in zebrafish. They found that injury-induced Notch activity peaks at 24 hours after injury but diminishes as the heart regenerates, so that by 96 hours it has returned to normal. If Notch is blocked, however, this prevents heart cell growth and stops heart precursor cells from reprogramming and maturing into cells that can replace the damaged cells.
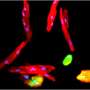
"Open annotations. The current annotation count on this page is 0. They next explored whether heart injury could alter blood flow forces and, in turn, control injury-induced Notch signaling. Klf2a is a molecule that responds to changes in blood flow and switches on certain genes in response. In regions of the injured heart where blood flow was most disrupted, they found that levels of Klf2a were increased. In addition, they found that levels of Klf2a overlapped with the levels of Notch.
Further experiments revealed that, when mutated, Trpv4—a molecule that is known to 'sense' changes in blood flow and can switch on the gene for Klf2a—led to a reduced amount of genes that drive heart cell growth and fewer cells maturing to replace the damaged tissue. Additionally, the team found that changes in blood flow controls heart cell reprogramming and growth via another two molecules, BMP and Erbb2. As these molecules are important for heart regeneration in mammals, the changes observed in the zebrafish may also hold true for other organisms, including humans.
"Our findings show how the heart senses and adaptively responds to environmental changes caused by injury, and provide insight into how flow-mediated mechanisms may regulate heart cell reprogramming and heart regeneration," concludes senior author Neil Chi, Professor of Medicine at UC San Diego. "Future studies are now needed to explore whether blood flow forces may affect mammals such as mice and to reveal new mechanisms that could take us a step towards being able to regenerate the human heart."
More information: Manuel Gálvez-Santisteban et al. Hemodynamic-mediated endocardial signaling controls in vivo myocardial reprogramming, eLife (2019). DOI: 10.7554/eLife.44816