Study illuminates serious but treatable lung autoimmunity in rare disease APECED
Autoimmune lung inflammation, or pneumonitis, is a common, early and often-overlooked symptom of the rare disorder APECED, a new NIAID-led study has revealed. If untreated, APECED pneumonitis can cause severe, life-threatening lung damage. The study results, published June 5 in Science Translational Medicine, illuminate the immune responses involved in APECED pneumonitis and provide early evidence for a promising treatment strategy.
APECED is a genetic disease that leads to defects in the autoimmune regulator (AIRE) protein, which helps teach immune cells how to distinguish the body's own cells and tissues from foreign invaders. People with APECED may experience a diverse range of symptoms, including autoimmunity against several organs and an increased susceptibility to chronic fungal infections of the mucous membranes and nails.
While previous studies had suggested that only a small subset of people with APECED develop lung autoimmunity, investigators led by NIAID's Michail Lionakis, M.D., Sc.D., found that 21 of 50 participants (42 percent) with APECED enrolled in a natural history study at the NIH Clinical Center had pneumonitis. Only one participant had been formally diagnosed with pneumonitis prior to enrollment in the NIH study. However, nearly all those with pneumonitis had experienced chronic respiratory symptoms such as coughing, and radiographic and other clinical tests showed evidence of abnormal lung function. In 8 of the 21 participants, pneumonitis developed early in the course of APECED, before other characteristic symptoms of the disorder became apparent.
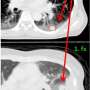
Although the presence of certain autoantibodies—antibodies that target the body's own tissues—correlates with APECED pneumonitis, the NIH researchers found that chest computed tomography (CT) was the most sensitive test for diagnosing this lung disease, including early cases in which respiratory symptoms had not yet developed. Due to the potentially fatal consequences of untreated pneumonitis, the researchers suggest that all patients with APECED should be evaluated with chest CT imaging.
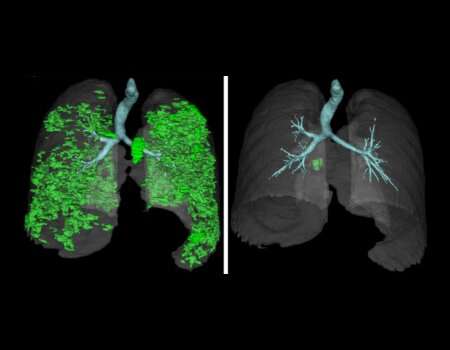
Further testing pinpointed the immune responses characteristic of APECED pneumonitis. Large numbers of activated neutrophils accumulate in the patient airways, while T cells and B cells infiltrate the lung tissue and drive progression of the disease. Experiments with mouse models of AIRE deficiency suggested that depleting T and B cells may be an effective strategy to treat APECED pneumonitis.
Based on these findings, NIH physicians gave five study participants combinations of existing medications that target T and B cells, a treatment that resulted in remission of their pneumonitis. The patients' chronic respiratory symptoms, such as cough and shortness of breath, resolved, and radiographic and lung function tests showed marked improvement. Treatment of a larger number of APECED patients with pneumonitis will be needed to validate these promising findings, the scientists note.
Overall, the findings draw attention to a previously largely unrecognized complication of APECED that can have life-threatening consequences and form a foundation for future clinical trials to assess the best therapy for people with this autoimmune lung disease. Additionally, these insights may have applications beyond APECED. The researchers identified similar clinical symptoms, lung-targeted autoantibodies and lung pathology in other diseases with thymic dysfunction and AIRE defects, including RAG deficiency and thymoma, a type of tumor originating in the thymus.
More information: Elise M. N. Ferré et al. Lymphocyte-driven regional immunopathology in pneumonitis caused by impaired central immune tolerance, Science Translational Medicine (2019). DOI: 10.1126/scitranslmed.aav5597