The growing need for bone marrow donors
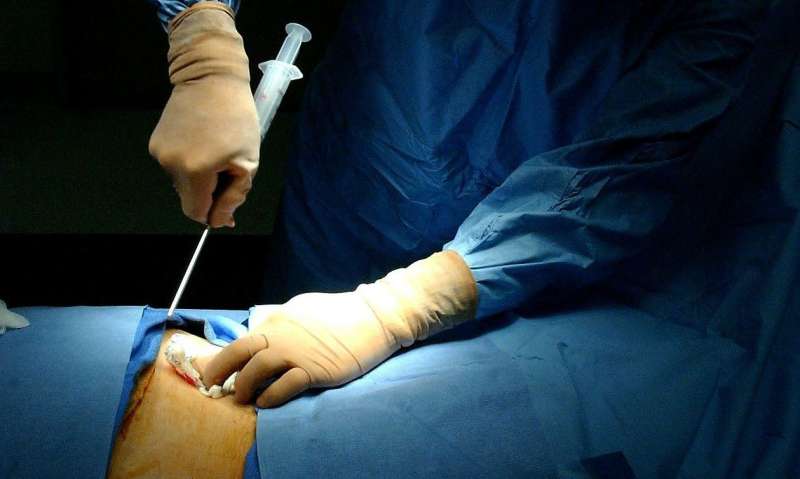
Close to 5,000 people in the U.S. undergo a bone marrow transplant annually. Also known as a stem cell transplant, this procedure replaces damaged or diseased bone marrow with healthy cells.
The process involves wiping out the body's bone marrow and immune system with chemotherapy and sometimes radiation. Then healthy donor cells are infused intravenously into the bloodstream so new cells can grow.
Bone marrow transplants often are used to treat leukemia; lymphomas; multiple myeloma; and other nonmalignant blood disorders, such as sickle cell anemia.
Finding A Donor
As with solid organ transplantation, the most important factor in a successful bone marrow transplant is finding a donor that is matched in terms of human leukocyte antigens (HLA).
"HLA stands for human leukocyte antigens, which are proteins or markers on the surface of the cells. "The body's immune system uses these markers to recognize which cells belong in your body and which do not," explains Dr. Ernesto Ayala, a Mayo Clinic hematologist/oncologist with the Bone Marrow Transplant Program. "We want the donor to be HLA identical with the patient or as close as possible. This is critical for the success of the transplant."
Typically, doctors look to a patient's family first for a match. "On average, we will find a donor in the patient's family only 20% to 25% of the time. And then there are patients who do not have siblings or children. The next best option is to go to the registry for a match," says Dr. Ayala.
Be The Match
For more than 30 years, an organization known as Be The Match has operated an international bone marrow registry that aims to match donors and patients in need. Mayo Clinic is one of the 152 transplant centers in the U.S. who partner with Be The Match. Although there are more than 12 million donors in the U.S., Dr. Ayala is passionate about growing the bone marrow donor registry, as finding a match is not always easy. "The biggest challenge we have in finding donors for patients needing bone marrow transplantation is ethnicity," he says.
"For a Caucasian American, the chance of finding an HLA-matched bone marrow donor through the international registry is around 75%. But if the patient belongs to an ethnic minority, let's say, African American or Hispanic or Middle Eastern, then the chance of finding a donor in the registry drastically drops to less than 25%, meaning many of these patients may never receive a transplant."
How To Become A Donor
Joining the donor registry is simple, says Dr. Ayala. "To become a bone marrow donor, you go bethematch.com; provide some demographic information, such as your age, gender and location; and request a kit. When you receive the kit, you swab your cheek, put it back in the envelope, seal it and send it. That's it."
Dr. Ayala says that if you are found to be a match for someone, you'll get a phone call. "They will say, 'We need you.' And then they will set up a time for you to come to a transplant center such as Mayo Clinic. You'll have a medical evaluation—reviewing your medical history, physical, some blood tests—just to make sure you are a healthy donor, and then you will be cleared for the donation."
The patient's medical team will decide if they prefer bone marrow extracted from the pelvis, which is performed in the operating room under general anesthesia, or a peripheral blood stem cell graft, which is an outpatient procedure.
In either case, donors are fully recovered and back to normal activity within 2-3 days. "I believe being a bone marrow donor is an act of generosity," says Dr. Ayala. "The more donors we have in the registry, the more donors we will have for our patients, especially for ethnic minorities. The need remains critical."
©2019 Mayo Foundation for Medical Education and Research
Distributed by Tribune Content Agency, LLC.