New frontier highlights role of smartphones in addressing Australia's mental health crisis
With smartphones and smart devices now ubiquitous in most Australian homes, a review by the Black Dog Institute has identified how these technologies can be used to identify, prevent and help treat mental illness.
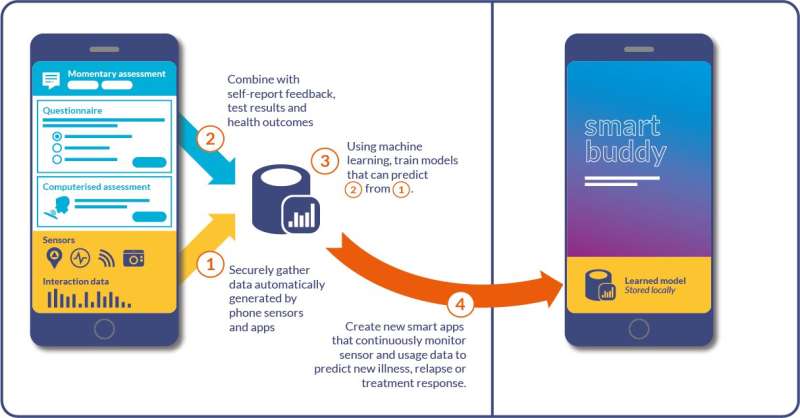
Published today in npj Digital Medicine, the review presents a vision for how data generated automatically and continuously by smart devices—such as smartphone-measured sleep continuity and typing fluency—can provide valuable information to mental health professionals about mental illness symptom severity and relapse.
The new science of 'digital phenotyping' uses data collected from smart devices to build a rich, personalised digital picture of behaviour, track markers of depression and anxiety, and develop new ways to diagnose illness, choose effective treatments and detect relapse before it occurs.
The principles of digital phenotyping are already being utilised by researchers across the world. Research conducted by researchers in Denmark is showing how smartphone technology can predict relapse amongst those living with bipolar disorder using changes in how calls and text messages are sent. Locally, Black Dog Institute has used machine learning to detect Twitter users who were at risk of suicide through the identification of suicide-related posts.
The review's lead author, Black Dog Institute's Research Fellow in Health Informatics, Dr. Kit Huckvale, said the idea that this data could be used to build a comprehensive picture of mental health is a potentially revolutionary concept.
"Today, clinicians and mental health researchers have an incomplete picture of what people experience before and during mental illness. This incomplete picture means real challenges for diagnosis, monitoring and knowing which treatments are likely to work," said Dr. Huckvale.
"Digital phenotyping helps us build an objective, high-resolution picture of behaviour that is more comprehensive than self-report information. Because smartphones are always carried and always on, we can collect this information unobtrusively and without creating a significant burden on individuals.
"Nobody wants to be defined by their illness. We know that people just want to get on with their lives. Imagine a smart app 'buddy' that shoulders the burden of keeping tabs on your condition and only pipes up when something changes. This is the kind of step change in self-management that digital phenotyping will allow."
In addition to providing thorough and unbiased data, the review outlines how those experiencing mental ill-health may also benefit from digital phenotyping when paired with personalised treatments and digital therapies.
"Based on how individuals interact online, digital phenotyping can be used to help tailor the advice and guidance offered by eHealth apps, or it can be used to tailor how an eHealth app looks and interacts with the individual," said Dr. Huckvale.
With the potentially positive implications for individuals experiencing mental ill-health, as well as for researchers and mental health professionals, Black Dog Institute is looking at ways of making digital phenotyping a widely accessible clinical tool that can help guide future research and treatments for mental ill-health.
A key component of the Black Dog Institute vision is the establishment of a Digital Phenotyping Bank—a new national resource that contains the signals from thousands of individuals. The Bank aims to accelerate collaborative research involving mental health specialists, computer science and machine learning experts, patient and public representatives and healthcare delivery organisations.
Black Dog Institute's Director and Chief Scientist and Interim Joint CEO of the Mindgardens Neuroscience Network, Scientia Professor Helen Christensen, says the development of a Digital Phenotype Bank is imperative to progress in mental health research.
"Like biobanks, a Digital Phenotype bank could help accelerate the pace of future breakthroughs, encourage cross-disciplinary collaboration, and aid in the building of robust datasets that will help us better understand the markers for mental illness onset and relapse" said Christensen.
"Encouraging the real-time exchange of information and partnership amongst researchers and mental health professionals will go a long way towards helping to deliver research and therapies that will truly affect change at a population level, which we hope will help quell Australia's growing mental health crisis."
More information: Toward clinical digital phenotyping: a timely opportunity to consider purpose, quality, and safety. npj Digital Medicine, DOI: 10.1038/s41746-019-0166-1