Medical management vs. mechanical thrombectomy for mild strokes: Same safety and effectiveness
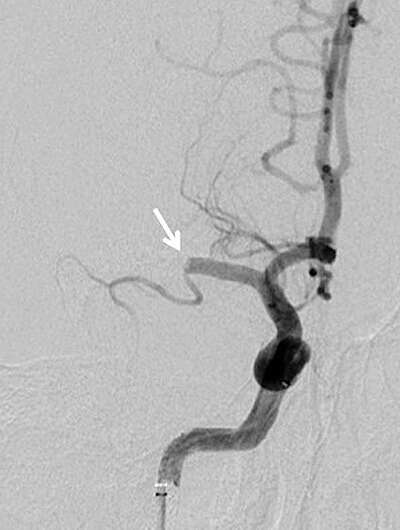
The use of clot retrieval devices to treat patients with ischemic stroke has risen steadily since the technology was first approved by the FDA nearly eight years ago. The minimally invasive procedure, known as mechanical thrombectomy, uses an X-ray guided device to physically remove a blood clot blocking a large vessel in the brain, thus restoring blood flow to the brain.
The endovascular treatment has proved life-saving for many patients with devastating strokes caused by emergent large vessel occlusions (ELVO) when administered up to 24 hours of symptom onset, said Max Mokin, MD, Ph.D., associate professor of neurosurgery and neurology at the University of South Florida Health (USF Health) Morsani College of Medicine. "Mechanical thrombectomy also has been shown to reduce disability in major strokes. We see less paralysis, speech problems and other stroke complications, faster recoveries, and less time needed in rehabilitation with these stroke survivors."
Dr. Mokin is among the co-investigators of a new international multicenter study and comprehensive meta-analysis, published Sept. 23 in JAMA Neurology, which compares best medical management to mechanical thrombectomy (with or without pretreatment with clot-busting drugs) for ELVO strokes classified as "mild." The study was led by the University of Tennessee Health Sciences Center.
While the safety and effectiveness of mechanical thrombectomy for treating moderate-to-severe ELVO strokes has been established, questions remain about its benefit for the subgroup of patients (up to 10 percent of all ELVO cases) experiencing mild stroke symptoms when evaluated in emergency departments. Would more conservative "best medical management" with intravenously administered clot-busting drugs like tissue plasminogen activator (tPA) or aspirin alone suffice for these cases, or can mechanical thrombectomy offer superior treatment?
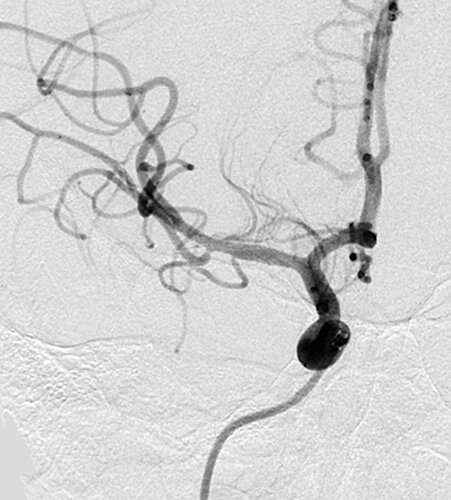
The retrospective study reported in JAMA Neurology found that overall both treatment approaches showed the same safety and effectiveness in patients with ELVO strokes who presented with milder symptoms—medical thrombectomy was neither more nor less beneficial. The paper's authors concluded that randomized clinical trials are needed to definitively evaluate the potential effectiveness of thrombectomy compared with medical management in patients with ELVO who exhibit mild neurological deficits.
The researchers pooled data from 16 high-volume endovascular stroke centers in North America, Europe and Asia, including USF Health's comprehensive stroke center at Tampa General Hospital. They analyzed the outcomes in 251 adult patients with mild ELVO strokes as scored by the standardized National Institutes of Health Stroke Scale, widely used by doctors to measure neurological symptoms such as impaired movement, visual field, facial droop and slurring of speech and to help determine appropriate treatment. The patients had received one of two treatment approaches: best medical management, or mechanical thrombectomy with or without pretreatment with clot-dissolving medications. The researchers then included this new retrospective study in a meta-analysis of three other outcomes studies comparing medical therapy with thrombectomy.
A lower rate of asymptomatic brain hemorrhage was found in the best medical therapy group, while the rate of functional independence three months after emergency treatment was higher in the medical thrombectomy group. However, their systematic review and meta-analysis of all four studies—the largest to date for this type of minor stroke—did not document any independent associations between the two treatment approaches and patient safety or effectiveness outcomes.
"This study does not answer our question about whether minor strokes should, or should not, be treated with mechanical thrombectomy in this particular patient population," Dr. Mokin said. "But, it does offer evidence that mechanical thrombectomy is as safe as medical therapy alone. Ethically, that can help us move forward with randomized patient trials to answer the question."
Dr. Mokin is the principal investigator for a three-year $419,000 grant from the NIH's National Institute of Neurological Disorders and Stroke, studying how patient brain vessel anatomy interacts with the clot removal devices. The goal is to optimize endovascular approaches for treating acute ischemic stroke, a leading cause of death and long-term disability worldwide.