New clinical research offers possibility of future rehabilitation for patients in vegetative, minimally conscious state
Non-invasive brain stimulation is to be trialled for the first time alongside advanced brain imaging techniques in patients who are minimally conscious or in a vegetative state.
The study builds on promising results from the Centre for Human Brain Health at the University of Birmingham which suggested that non-invasive brain stimulation can improve the success of rehabilitation for non-responsive patients.
The RAINDROP trial, a collaboration between the University of Birmingham and The Wellington Hospital, part of HCA Healthcare UK, will use advanced brain imaging technologies to track the effects of non-invasive brain stimulation in a small group of patients. The aim is to better understand how stimulation techniques can be harnessed to improve communication and recovery, with the hope of one day offering improved rehabilitation rates for non-responsive patients with a prolonged disorder of consciousness.
The RAINDROP trial
Improvements in trauma care have increased the chances of surviving the most severe brain injuries. Recent research has shown that as many as 20% of these patients retain a much higher level of awareness than could be expected from their clinical diagnoses—however, these patients remain unable to demonstrate their awareness, trapped in their unresponsive bodies.
Previous research by the Centre for Human Brain Health at the University of Birmingham and Western University, Canada, pinpointed what happens in the brain to cause this unresponsive behaviour—suggesting for the first time a potential target for treatment.
In the RAINDROP study, researchers will work with five patients in The Wellington Hospital's Prolonged Disorders of Consciousness Unit (PDoCU) to examine how a form of brain stimulation called transcranial direct current stimulation (tDCS) can be used to identify and treat damaged connections within the brain.
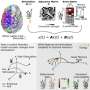
During the treatment, low levels of direct current are targeted at specific areas of the brain via electrodes placed on the patient's head. The current is applied to a region at the top of the brain responsible for motor control, and also directed at the thalamus, a region deep inside the brain which relays motor signals and controls consciousness.
While the stimulation is delivered, researchers will use multimodal brain imaging, to measure the effect on brain function. These techniques include functional magnetic resonance imaging (fMRI) which looks at changes in blood flow to measure activity in different areas of the brain, and electrophysiology, which measures the electrical activity generated by neurons as they fire in the brain.
Dr. Davinia Fernández-Espejo of the Centre for Human Brain Health at the University of Birmingham, is leading the study, which builds on earlier work carried out in healthy subjects, funded by the Medical Research Council.
Dr. Fernández-Espejo says: "The different areas of our brain need to have good connections between them in order to carry out different functions. By finding the right ways to stimulate this network, we're able to improve these connections, helping the brain to compensate for the damaged pathways, and improve the patient's ability to respond."
"We've already been able to show that these techniques have potential among healthy subjects. This important next step will enable us to test their effect among patients."
Dr. Antonio Incisa, Lead Clinical Neuropsychologist and Principal Investigator at The Wellington Hospital Prolonged Disorders of Consciousness Unit, says: "With RAINDROP we hope to further our understanding of how stimulating certain areas of the brain using non-invasive techniques can lead to improvements in rehabilitation for patients. This will ultimately open the way for us to establish research in neuroscience applied to neurological rehabilitation at The Wellington Hospital."
Eric Reichle, Chief Executive of the Wellington Hospital, says: "At the Wellington Hospital, we feel incredibly privileged to be involved in such an important research programme. Improving patient outcomes is dearly important to everything we do, so we have high hopes about how the findings can shape care and improve rehabilitation for patients."
The RAINDROP study is the first step of a long-term collaboration between Dr. Fernández-Espejo and Dr. Damian Cruse at the Centre for Human Brain Health and the Prolonged Disorders of Consciousness Unit at The Wellington Hospital to investigate novel bedside methods for diagnosis and rehabilitation in prolonged disorders of consciousness. If successful, the study will inform a large clinical trial that will recruit patients from multiple specialised centres across the UK.
The study was announced today at the 'Prolonged Disorders of Consciousness: From Scientific Discovery to Clinical Practice' conference.