Study maps landmarks of peripheral artery disease to guide treatment development

Novel biomedical advances that show promise in the lab often fall short in clinical trials. For researchers studying peripheral artery disease, this is made more difficult by a lack of standardized metrics for what recovery looks like. A new study from University of Illinois at Urbana-Champaign researchers identifies major landmarks of PAD recovery, creating signposts for researchers seeking to understand the disease and develop treatments.
"Having these landmarks could aid in more optimal approaches to treatment, identifying what kind of treatment could work best for an individual patient and when it would be most effective," said Illinois bioengineering professor Wawrzyniec L. Dobrucki, who led the study. He also is affiliated with the Carle Illinois College of Medicine.
PAD is a narrowing of the arteries in the limbs, most commonly the legs, so they don't receive enough blood flow. It often isn't diagnosed until walking becomes painful, when the disease is already fairly advanced. Diabetes, obesity, smoking and age increase the risk for PAD and can mask the symptoms, making PAD difficult to diagnose. Once diagnosed, there is no standard treatment, and doctors may struggle to find the right approach for a patient or to tell whether a patient is improving, Dobrucki said.
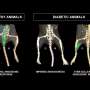
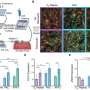
The researchers used multiple imaging methods to create a holistic picture of the changes in muscle tissue, blood vessels and gene expression through four stages of recovery after mice had the arteries in their legs surgically narrowed to mimic the narrowing found in PAD patients. They published their results in the journal Theranostics.
"There are a lot of people who study PAD, so there are all these potential new therapies, but we don't see them in the clinics," said postdoctoral researcher Jamila Hedhli, the first author of the paper. "So the main goal of this paper is utilizing these landmarks to standardize our practice as researchers. How can we see if the benefit of certain therapies is really comparable if we are not measuring the same thing?"
Dobrucki's group collaborated with bioengineering professor Michael Insana, chemistry professor Jefferson Chan and senior research scientist Iwona Dobrucka, the director of the Molecular Imaging Laboratory in the Beckman Institute for Advanced Science and Technology, to monitor the mice with a suite of imaging technologies that could be found in hospitals or clinics, including ultrasound, laser speckle contrast, photoacoustics, PET and more. Each method documented a different aspect of the mouse's response to the artery narrowing—anatomy, metabolism, muscle function, the formation of new blood vessels, oxygen perfusion and genetic activity.
By serially imaging the mice over time, the researchers identified key features and events over four phases of recovery.
"Each imaging method gives us a different aspect of the recovery of PAD that the other tools will not. So instead of looking at only one thing, now we're looking at a whole spectrum of the recovery," Hedhli said. "By looking at these landmarks, we're allowing scientists to use them as a tool to say 'At this point, I should see this happening, and if we add this kind of therapy, there should be an enhancement in recovery.'"
Though mice are an imperfect model for human PAD, each of the imaging platforms the researchers used can translate to human PAD patients, as well as to other diseases, Dobrucki said. Next, the researchers plan to map the landmarks of PAD in larger animals often used in preclinical studies, such as pigs, and ultimately in human patients.
"We are very interested in improving diagnosis and treatment," Hedhli said. "Many people are working to develop early diagnosis and treatment options for patients. Having standard landmarks for researchers to refer to can facilitate all of these findings, move them forward to clinic and, we hope, result in successful clinical trials."
More information: Jamila Hedhli et al, Imaging the Landmarks of Vascular Recovery, Theranostics (2020). DOI: 10.7150/thno.36022