Study predicts COVID-19's impact across Africa
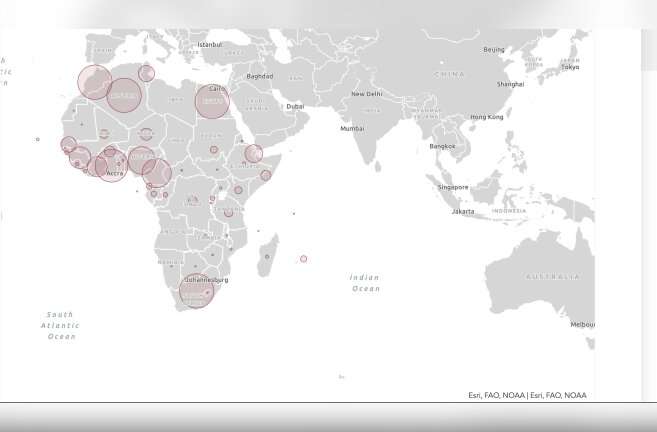
As of April 30, there were approximately 39,000 reported cases of COVID-19 in Africa. But public health officials fear it will only be a matter of time before infections start to rise on the world's second largest continent, which is home to 1.3 billion people.
In response to the looming pandemic threat, a team of African scientists—including Yale School of Public Health alumna Uzma Alam, Ph.D., MPH—worked around the clock in recent weeks to develop one of the first pandemic models forecasting COVID-19 infection and mortality rates across Africa.
The researchers used advanced data science to ensure their projections accounted for existing socioeconomic conditions in different African countries. The resulting forecast provides important region-specific data that is intended to help policymakers and healthcare systems prepare for potential outbreaks.
Alam, a global health specialist with the Africa Institute for Health Policy Foundation in Kenya, discussed the study's key findings.
What impact do you expect COVID-19 to have in Africa?
UA: Epidemiologically, Africa has lagged behind the rest of the world with a later introduction of SARS-CoV-2, the virus that causes COVID-19. Yet our research shows the spread of the disease is rapidly changing. We found that in the absence of appropriate policies, the African continent is likely to experience catastrophic levels of COVID-19. By June 30, 2020, we estimate that as many as 16.3 million people in Africa could contract COVID-19. We project a 135% increase in incidence of COVID-19 from April to May and a 39% increase from May to June. Our models show Northern Africa will be most affected by the pandemic and Eastern Africa will be the least affected. Hotspots will include Morocco and Algeria in the North; Zambia and Djibouti in the East; and Ghana and Cote d'Ivoire in the West. The Democratic Republic of the Congo and Gabon will be hotspots in Central Africa while South Africa and Swaziland will have significant infection rates in the South.
Will certain areas of Africa be hit harder than others?
UA: Our model forecasts that the population level prevalence of COVID-19 in Africa is expected to remain under 1.5% throughout the three-month prediction period, April-June. However, there are wide interregional differences. For example, in the Northern and Southern Africa subregions, cumulative infection rates are expected to be slightly over 3 % with the rate in the other subregions expected to be around 3.5% as of June 30. This implies that certain areas in Africa will indeed be hit harder compared to others. Moreover, these subregional and country-level differences are expected to deepen as the pandemic becomes more established in Africa. The reason behind these differences is something our model focused on. We wanted to understand the factors that accelerate and mitigate the spread and mortality of COVID-19, while accounting for local realities. These factors include the strength of local healthcare systems, burden of other infectious diseases such as HIV, socioeconomic status and population levels. We found that less urbanized countries with low levels of socioeconomic development (hence, fewer connections to the rest of the world), are likely to experience lower and slower disease transmissions in the early stages of the epidemic. However, those same factors that initially work to those countries' benefit can hinder interventions that have lessened the impact of COVID-19 elsewhere.
Your study mentions that COVID-19 prevention measures may be difficult to implement in some parts of Africa. Can you please elaborate?
UA: Large-scale prevention measures that have worked in other countries such as frequent hand washing, limiting movement and social distancing are not enough, or at best impractical for addressing the pandemic in the African context. Barriers to such measures include (a) large informal settlements (b) lack of appropriate water and sanitation and (c) high concentrations of marginalized communities, including approximately 12.3 million forcibly displaced people and 4.2 million refugees. Therefore, in the African context, it is imperative that response measures be contextualized to address underlying individual and structural factors that are likely to complicate a strategic response. Interventions also must be balanced with the need to maintain individual livelihoods and social cohesion. For instance, workers who lose their jobs in urban areas due to economic lockdowns are likely to move back home to rural areas where large elderly populations reside, heightening health risks. Consequently, measures such as the provision of adequate water and sanitation subsidies, reliable food distribution and targeted restrictions of movement (e.g. from urban to rural) would go a long way to mitigating spread.
Are Africa's healthcare systems adequately prepared for this pandemic?
UA: Africa in general has weak health systems and the reasons behind this are wide ranging—from poor governance to Africa being forced to adopt free-market models of economic austerity under the International Monetary Fund's structural adjustment programs. These policies unfortunately have a deleterious effect. We need only look back to the 2014 Ebola epidemic to see how an estimated additional 11,000 deaths occurred due to weak health system infrastructures. During this pandemic, we are seeing far more developed health systems, such as those in the United States and United Kingdom, being overstretched. Therefore, it is likely that Africa's already strained healthcare system is going to be overburdened by COVID-19. However, Africa has the benefit of having learned from past epidemics like Ebola. As a result, local leadership among African nations is already taking appropriate steps, from the development of local testing kits to the production of locally-sourced ventilators. What impact the strength of local healthcare systems ultimately will have on the pandemic remains unknown. Our team is currently conducting a systematic analysis of healthcare systems in Africa and we will make our findings publicly available when they are ready.
What steps does Africa need to take to control the spread of COVID-19?
UA: Understanding the factors that accelerate and those that mitigate the spread and mortality of COVID-19, while accounting for local realities, is fundamental for sound public health measures to tackle this pandemic. Regional initiatives are already engaging with our findings, as the first systematic projections accounting for local context. Lessons from HIV/AIDS programming have taught us that highly effective health interventions fail if the local context is not recognized. Secondly, some of the most effective responses to global health threats involve multi-stakeholder partnerships. Fortunately, many African health systems have implemented such partnerships in the past. They would be best served to leverage that experience and those shared resources again in responding to COVID-19. African policymakers should also consider the impact certain interventions may have in deepening health inequalities. We recommend they use data-driven approaches to identify vulnerable groups so they can be properly and equitably supported during this crisis. At a time of a pandemic, no single community should be marginalized. Finally, in as much as health systems are dealing with an emerging situation, data is fundamental in delivering an evidence-based response. We have made sure our forecasting model is comprehensive, yet agile enough to be regularly updated as circumstances demand.
A pre-print version of the study, "COVID-19 pandemic in the African continent: Forecasts of cumulative cases, new infections, and mortality," which has not undergone peer review, can be found on MedRxiv.
More information: Tom Achoki et al. COVID-19 pandemic in the African continent: Forecasts of cumulative cases, new infections, and mortality, MedRxiv (2020). DOI: 10.1101/2020.04.09.20059154



















