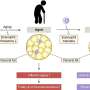
Influenza A virus directly modulates eosinophil responses
Eosinophils residing in the airways of mice respond to influenza A virus (IAV) infection through alterations in surface expression of various markers necessary for migration and cellular immunity responses, according to research published in the Journal of Leukocyte Biology by researchers from Le Bonheur Children's Hospital and the University of Tennessee Health Science Center.
Previous research explored the effects of IAV infection in patients with allergic asthma. During the 2009 influenza pandemic, patients hospitalized with influenza experienced lower morbidity if allergic asthma was an underlying condition. In mice, the researchers reported that the beneficial effect of this co-morbidity correlated with a dramatic increase in eosinophils in the airways, which is a hallmark of allergic asthma. Eosinophils were susceptible to IAV infection and also presented IAV antigens to CD8+ T-cells which are heavily involved in resolving viral infections.
This implied that eosinophils actively contribute to the antiviral response during influenza. While once considered to be a cell that degranulated after allergen encounters and incidentally promoted host pathology during allergy, this research contributed to expand the role of eosinophils to that of anti-viral mediators and specifically showed that eosinophils are active participants in the resolution of influenza. Many of processes that cumulate in eosinophils making this valuable contribution are unclear.
"Very little is known about how eosinophils respond to direct exposure to IAV or the microenvironment in which the viral burden is high," said Le Bonheur and UTHSC researcher Amali Samarasinghe, Ph.D. "We hypothesized that eosinophils would dynamically respond to the presence of IAV through phenotypic, transcriptomic and physiologic changes."
Researchers investigated eosinophil characteristics in different niches in mice using a mouse model of fungal asthma and influenza, in addition to responses when exposed to IAV in vitro.
Results of the study included the following:
1. Mice with fungal allergic asthma have a lower pro-inflammatory cytokine profile in their lungs during influenza than non-allergic mice.
2. Eosinophil surface antigens are differentially regulated in mice with fungal asthma and influenza. During influenza, eosinophils changed the surface expression of proteins involved in antigen presentation, activation and survival depending on both niche and allergic environment.
3. Following virus exposure, a discrete subset of eosinophils that decreased their surface expression of Siglec-F were also more active. Siglec-Flo expressors also increased expression of eosinophil survival receptor IL-5R and downregulated CD62L which is associated with activation. These data suggest that subpopulations of eosinophils may have differing functions during IAV infection.
4. IAV exposure alters the eosinophil transcriptome. IAV-infected eosinophils reduced overall transcriptional activity but up-regulated transcription of mRNAs encoding viral recognition proteins.
5. Eosinophils reduce mitochondrial respiration in response to IAV. Eosinophils had a lowered basal respiration rate and an overall reduction in mitochondrial respiration.
6. Flu-PB-1 pulsed eosinophils promote the generation of cytotoxic CD8+ T-cells by causing demethylation of the Tbx21 locus. IAV-exposed eosinophils can communicate with CD8+ T-cells, resulting in epigenetic changes that allow the differentiation of IAV-specific CD8+ T-cells into effector cells.
Overall, mice with fungal asthma that were protected from severe IAV morbidity had reduced levels of cytokines—which can contribute to pathology when present in excess. When exposed to IAV, eosinophils initiate self-preservation mechanisms to survive viral infection, such as conserving energy by reducing transcription activity and mitochondrial respiration. Concurrently, they increase their ability to recognize IAV and induce epigenetic changes in CD8+ T-cells that initiate their differentiation into cytotoxic cells known to be a critical component of the antiviral response.
"Our research shows that eosinophils respond dynamically to IAV infection and contribute to antiviral host defense mechanisms during influenza" said Samarasinghe. "This information is important for selecting effective therapeutics for asthmatics that may benefit from eosinophil presence in airways during IAV infection."
More information: Kim S. LeMessurier et al, Influenza A virus directly modulates mouse eosinophil responses, Journal of Leukocyte Biology (2020). DOI: 10.1002/JLB.4MA0320-343R